Why is Switzerland behind in palliative care?
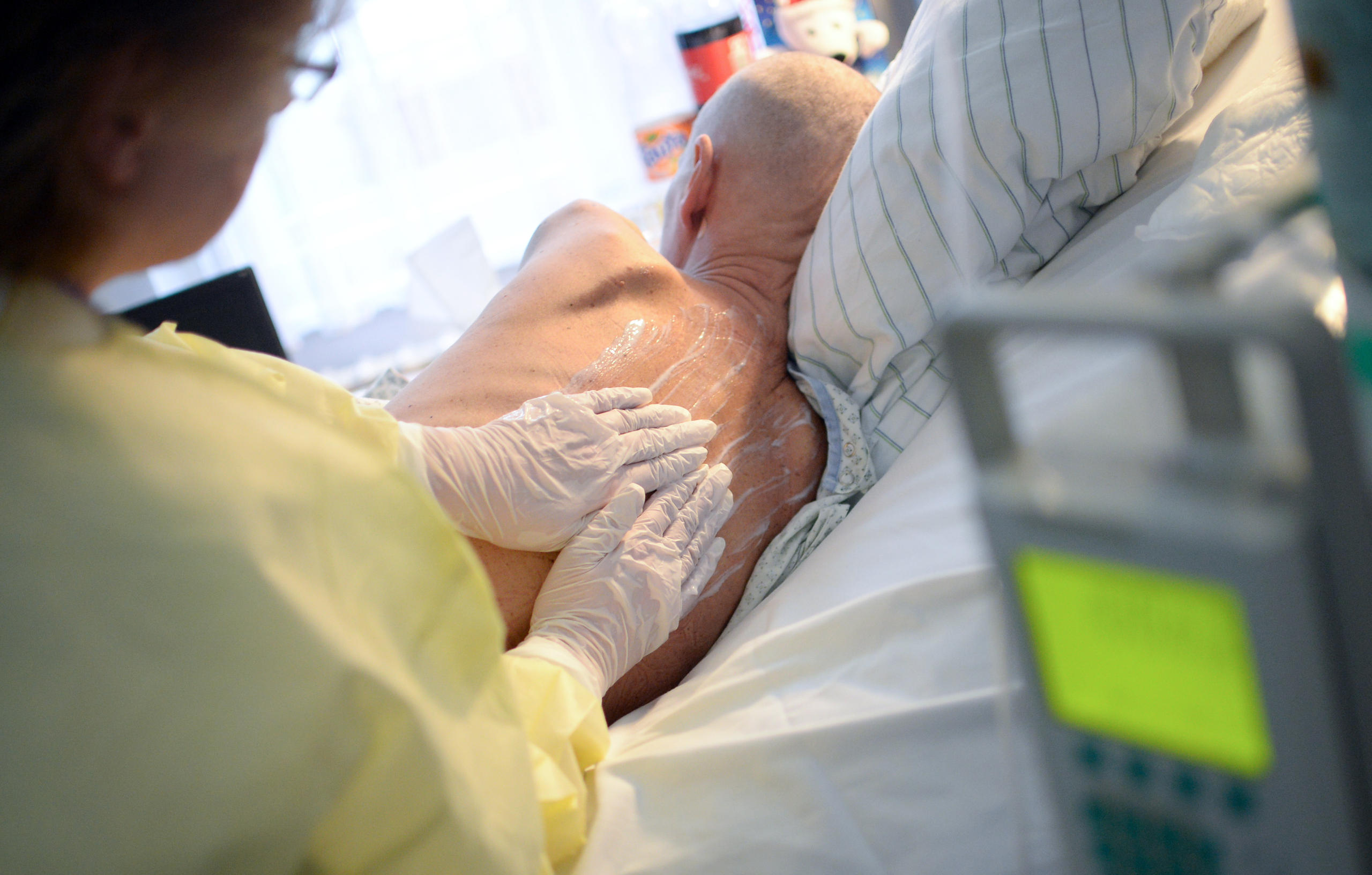
Switzerland has a short history of encouraging palliative care, with more awareness of curative treatment, acute care and assisted suicide as end of life options. But the appointment of a new university professorship on palliative care could help turn things around.
Earlier this year, Steffen EychmüllerExternal link was appointed Professor of Palliative Care External link– only the second such position in Switzerland – at the University of Bern. swissinfo.ch met him at the Centre for Palliative CareExternal link at the University Hospital Bern, which he heads.
It is clear that the experienced doctor is passionate about his job. The need for palliative careExternal link – well-planned multidisciplinary support for terminally ill patients and their families – will increase, given the ageing population. And so will the costs of this care. But these can be lowered if palliative care is properly planned, as is the case in countries like Australia and the United Kingdom.
swissinfo: Why is Switzerland behind other countries in terms of palliative care?
Steffen Eychmüller: There is a strong interest and emphasis on acute care and healing curative treatment. We have fantastic access to the most expensive and best technological possibilities for prolonging life in Switzerland.
Also, there has not been so much focus on the whole chronic care approach and living with an illness. This is possibly because we have a fragmented health care system: with hospitals as economic entities, long term care through nursing homes mostly paid out of pocket and home care. Switzerland has very few hospices. The expectation is that health problems can be managed and cured by fantastic hospital care and there is no sole responsibility for the whole range of health network institutions, like in a national health service.

The second Economist report about the quality of deathExternal link in different countries showed that last year Switzerland improved a little from position 19 to 15External link. But this rating shows that others [the United Kingdom, Australia] are better. These higher rated countries tend to have national health services.
swissinfo: What else do these countries have, which Switzerland doesn’t, in terms of palliative care?
S.E.: Experience. In countries like the United Kingdom, there is a 30-year-history of development of palliative care and people accept it. In Switzerland palliative care came in very late, in last six years, but I’m optimistic that in time it will also be established on a far more normal basis and also that patients and families think it’s not the end of all hope but a fantastic offer to get good quality of care.
swissinfo: So one might say that death, the end of life, this is still a bit of a taboo in Switzerland?
S.E.: It’s not a taboo in Switzerland because the media – and politicians – are very much concerned about the physician assisted suicide debate. It’s all about autonomy and how to end life in dignity and of course if you don’t have very good examples of how you can end your life with dignity in big institutions like hospitals, then you are happy that you have another option like physician assisted suicide.
Many see it as death through Exit or physician assisted suicide versus suffering endlessly in today’s healthcare. But this attitude might change if you see the opportunity to create, with your friends and family and the professionals, a vision for your end of life in dignity – and supported by palliative care.

More
Switzerland, leading the way in assisted suicide?
swissinfo: So would you say that because assisted suicide is quite widely accepted in Switzerland, this has interfered with people’s view of palliative care?
S.E.: I can only see it from the viewpoint that we are mostly asked to participate in public discussions comparing palliative care with physician assisted suicide, also because it promises more impassioned debates.
But I think it’s a very limited view of what should and could be end of life in our society. In Asia the end of life is regarded the peak of our life and there is a high level of respect for all those people entering the late phase of life. Back in Switzerland it is not regarded as being the best part of your life and is not given the highest level of worth and dignity.
Assisted suicide
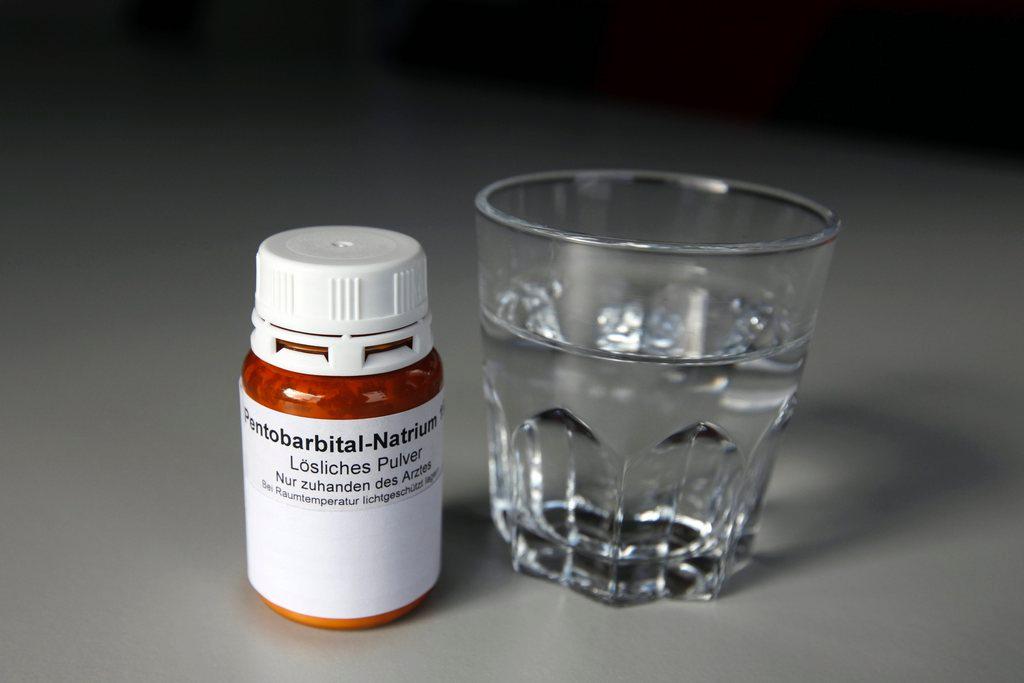
Swiss law tolerates assisted suicide when patients commit the act themselves and helpers have no vested interest in their death. It is mostly carried out through organisations such as Dignitas and Exit.
Physician-assisted suicide, but not euthanasia, is legal in Switzerland. A study published earlier this year found that in 2013, four out of five expected deaths, some form of medical end-of -life practice was carried out by doctors in German-speaking Switzerland. This was usually stopping or foregoing treatment; sometimes increasing painkillers like morphine. In the vast majority of cases this was done in agreement with the patient and his family.
swissinfo: What can be done in terms of promoting palliative care? An overarching national strategy does not seem realistic given the fragmented nature of health care system here.
S.E.: You are right and this is a political question and we as care providers can’t influence this much. It’s clear that in national health services, responsibility for all parts of health system is far higher. I think palliative care could go towards a more mixed system: so we have chronic care incentives for creating networks, a more national style healthcare system, but we maintain acute healthcare when needed. So we could take the best of both systems.
swissinfo: What motivated you personally to enter palliative care?
S.E.: It’s an incredible part of medicine, where you can really do human medicine. You are very much concerned with all the medical problems and details and sometimes it’s really very complex. On the other hand, you have the person, their life story, the family and you try to find the best way through this situation together.
People are always surprised that those working in palliative care are not sad, that burnout is a very rare phenomenon. So there is something in it which is meaningful for us too. So it’s not just superficial and I think this is a privilege.
The professorship
Steffen Eychmüller has been University of Bern chair in Palliative Medicine since February 1, 2016. It is the only position of its kind in German-speaking Switzerland. The second one is in Lausanne. The CHF3 million ($3.2 million) Bern position is being financed by the Swiss Academy of Medical SciencesExternal link and the health insurance HelsanaExternal link. Eychmüller said the position nevertheless remained independent.
Eychmüller says that in terms of the Swiss national strategy for palliative care, started six years ago, it’s quite a success to have a second professorship. He says it must be followed by chairs and academic positions for people with other professional backgrounds like social work and psychology. He says Switzerland is still “a developing country” in terms of having an international level of palliative care.
The national strategy lasted from 2010-2015. A national platform for palliative care will be launched External linkat the beginning of 2017, the Federal Health Office confirmed to swissinfo.ch. Its aim is to promote coordination and exchange between the various actors in palliative care. Issues such as financing and specialised palliative care in long-term institutional facilities will also be discussed with a view to finding solutions. “Everyone should have palliative care available to them at the end of their lives,” the health office said.
How is palliative care viewed in your country? Write in and let us know.

In compliance with the JTI standards
More: SWI swissinfo.ch certified by the Journalism Trust Initiative



You can find an overview of ongoing debates with our journalists here. Please join us!
If you want to start a conversation about a topic raised in this article or want to report factual errors, email us at english@swissinfo.ch.