Malaria: what the future holds

Last year to great acclaim, scientists cracked the genetic codes of both the deadliest malaria parasite and the mosquito that spreads it.
Every single day since then, at least 820,000 people have come down with the disease.
“The genome is a tremendous information source,” says Robert Ridley of the World Health Organization’s tropical disease research programme.
“However, I don’t think we should underestimate the difficulty of converting that knowledge into new tools – whether drugs, vaccines, insecticides or even transgenic mosquitoes.”
Fatal delay
Tweaking the mosquito to make it less able to transmit malaria may make sensational headlines but many experts believe that much of the current burden of malaria could be prevented with existing affordable interventions.
“There are grounds for hope,” says Hassan Mshinda, director of the Ifakara health research and development centre in Tanzania.
“Just by training mothers to recognise early symptoms and treatment, one can reduce malaria deaths.”
Traditional healers in Tanzania frequently treat a children’s illness characterised by fever and convulsions, called degedege.
Unfortunately, it shares many symptoms with malaria and if the child is suffering from the latter, the delay in treatment can be fatal.
In St Francis’ Hospital, Ifakara, four-year-old Lucrezia – who is suffering from cerebral malaria – has been lying in a coma for a month.
When she began suffering from convulsions, high fever, diarrhoea and shivering, her mother contacted traditional healers and only brought her to hospital after they had failed to produce results. By then it was too late to treat the malaria effectively.
Training traditional healers to distinguish degedege from malaria at an early stage and act upon that knowledge, resulting in a loss of business, is just another part of the equation.
Fresh challenge
A new study in Ifakara has shown that if young children are given a single dose of an antimalarial drug when they have their routine vaccinations, rates of anaemia are cut by at least 50 per cent.
“It proved to be outstandingly effective in reducing the malaria burden of these children because it happens in the first year of their lives which is the period of greatest risk,” says Christian Lengeler of the Swiss Tropical Institute.
“Combined with insecticide-treated nets, we now really have the means to make an impact on malaria.”
Some experts, however, have expressed concern that success with bed nets and intermittent therapy could pose new problems. By reducing the number or severity of attacks, you might lower the partial immunity acquired with age, making people more susceptible later in life.
“It means that we are in for the long term,” agrees Lengeler. “If you have a new generation of children with reduced immunity, you have to make sure that the children don’t get exposed later on to high levels of transmission.”
Affordable drugs
Tourists going on safari buy expensive, new medication while an African child dies of malaria every 30 seconds after second-rate treatment or no treatment at all.
Studies show that people in the poorest and rural areas simply do not get access to effective drugs.
“There is now a lot of international dynamism towards assisting sub-Saharan African countries to do something about malaria,” says Professor Zul Premji, head of the department of parasitic infections at the Muhimbili University College of Health Sciences in Dar es Salaam, Tanzania.
“But are we really reaching the target or are we just scratching the upper layers of the population? The whole issue is very closely tied to poverty alleviation.”
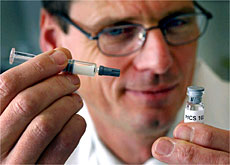
With growing resistance to existing drugs, there is an urgent need to discover new drugs at affordable prices for poor, disease-endemic countries.
“When you say a drug is not efficacious anymore, you have to produce an alternative and most of them are very expensive,” says Mshinda.
“Affordability is a major challenge. Most African countries are facing difficulties in changing their treatment policies simply because of the cost of the drugs.”
Child killer
HIV/Aids has shifted attention away from malaria completely. Yet in Tanzania, malaria remains the biggest health problem and is still the main killer, especially of children.
In research too, the malaria parasite is infinitely more complicated than the virus that causes Aids but it only receives about a tenth as much funding for research.
“If you imagine that there are 500 million cases of malaria each year and you’re talking about $1-2 per treatment to cure those people, then you’re talking of $1 billion a year,” says Ridley.
“To have a real impact on malaria control, you’re talking about billions of dollars.”
Governments can help create a conducive environment. They can put the proper regulatory mechanisms in place for drugs and insecticides, waive duties on mosquito nets, register products, assure quality and promote healthy behaviour.
To date less than half of the 44 African countries most affected by malaria have removed taxes on mosquito nets – a relatively simple step.
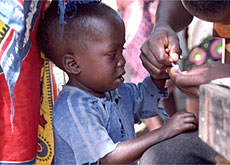
Malaria kills 3,000 African children every day despite the fact that the disease can be prevented and treated.
“We have the tools and the strategies,” says Lengeler. “We have to have the courage and determination to start today.”
swissinfo, Vincent Landon
In Africa, 3,000 children die of malaria every day.
New, effective drugs are not available for most of those who need them.
Few of the children at risk are protected by insecticide treated nets.
WHO says it is possible to halve the global burden of malaria by 2010.
Greater investment and political commitment is needed.

In compliance with the JTI standards
More: SWI swissinfo.ch certified by the Journalism Trust Initiative
You can find an overview of ongoing debates with our journalists here. Please join us!
If you want to start a conversation about a topic raised in this article or want to report factual errors, email us at english@swissinfo.ch.