Alternative therapies are put to the test
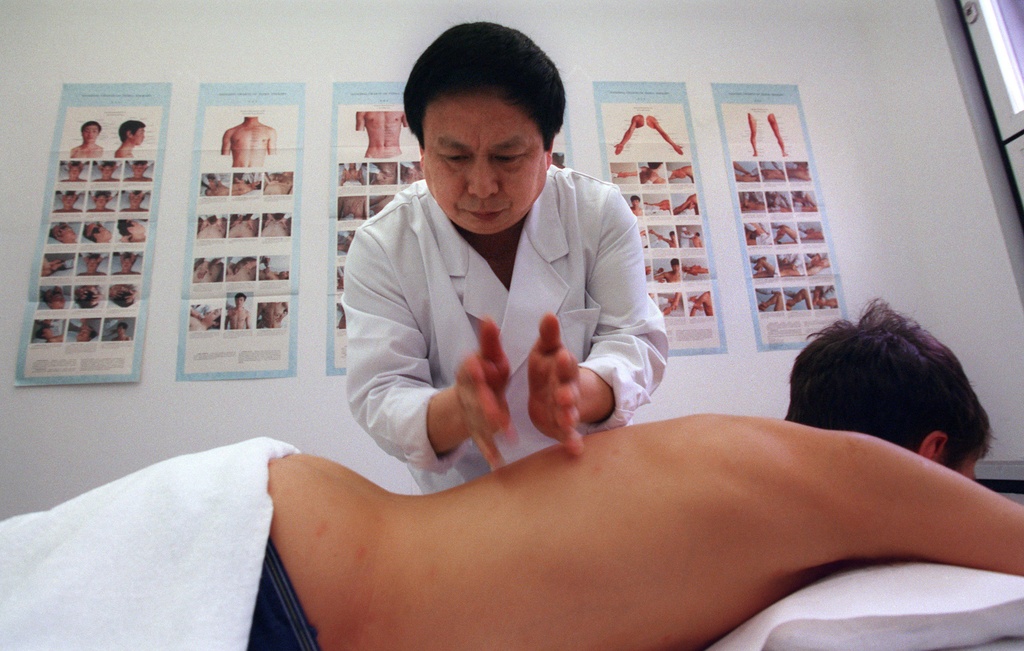
The Swiss government has given complementary medicine a second chance to prove its worth as an insurable health cost.
Interior Minister Didier Burkhalter has announced five therapies previously struck off the state insurance list will be reimbursable from 2012 as part of a six-year trial period. The sting: all must prove their “efficacy, cost-effectiveness and suitability” by 2017.
Back in 2005 the interior ministry rejected the therapies, arguing they failed to meet the legal requirement of “scientific proof” of the three efficacy criteria.
The reversal in policy follows a nationwide vote in 2009 in which two-thirds of Swiss backed including the therapies on the constitutional list of paid health services. It also takes into account an opposing recommendation by a federal commission in December to strike them permanently from the list because of a lack of scientific evidence.
For the new trial, providers of homeopathy, holistic, herbal and neural therapies and traditional Chinese medicine will have to evaluate their effectiveness. The findings will then go before a recognised international institute – still to be determined – that will provide an independent scientific assessment.
The medical establishment praised the decision to put the case before international scientific scrutiny while complementary medicine proponents welcomed the chance for “fair” assessments.
Ignazio Cassis, national vice-chairman of the Swiss Medical Association, said it was a “very wise and pragmatic” move as it left the decision up to the international scientific community, rather than the government or the Swiss population.
It will take advantage of international developments in medical science and better inform a decision on the issue in six years, he noted.
“It’s the law”
The outcome remained open, Jean-Marc Crevoisier, head of communications at the interior ministry, told swissinfo.ch.
“Until now we have not been able to prove fully that these five therapies are efficient, cost-effective and suitable. Some do it more than others.”
“The goal of these six years is to fill in the gaps for those that don’t manage to [meet these criteria] or do so only partially. We’ll see what happens, we cannot prejudge the results.”
The scientific testing will be done according to a mandate and standards fixed by the government, he explained.
“We must prove these three criteria to accept a therapy in the list for reimbursement. It’s required by the law.”
He noted that it was an “emotional” issue and the six-year trial period was set in order to examine the issue in the “most correct way possible”.
The government’s proposal also includes provisions to boost research and training in the field, which Crevoisier said would not be counter-productive, even if there is a negative result for the therapies after the trial.
International scrutiny
The government is now considering which international institute to approach. It could be a state-sponsored body such as the United States’s lead agency for scientific research on complementary medicine, the National Center for Complementary and Alternative Medicine. The National Institute of Clinical Excellence in Britain has been name-checked by others.
“The idea is that an international body evaluates existing studies adequately and they do not draw up new studies. That would not be possible in this timeframe. Many studies have been done already. The point is to assess them fairly,” said Hansueli Albonico, president of the federation of Swiss societies of complementary medicine.
He noted there was already evidence of the cost-effectiveness of the medicines, so it came down to the question of efficacy.
Fair hearing
Practitioners were “confident” in the outcome, he noted, “if we have the chance to convey solid facts from existing scientific studies – of which we have already 2,000 clinical trials – and if these contribute to a fair assessment”.
“I really welcome this move towards the international arena. I see this as a great opportunity.”
“In Germany, for example, the medical profession has been engaged in a dialogue for the past decade on pluralism in medicine and applying different methods – always with a view to effectiveness, appropriateness and efficiency.”
Switzerland has the highest number of practitioners per capita in the world – 17,200 registered with health insurers – this due notably to the various insurance packages covering complementary medicine.
He said the time had now come to widen the terms of reference for medicine.
“We need a shift away from methods used for testing effectiveness, such as are appropriate for drugs, to studies that show the overall benefit provided by these [complementary] methods,” he concluded.
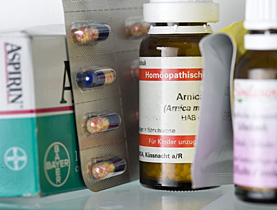
Homeopathy: Treatment involves giving a patient small amounts of drugs that, in larger quantities, cause symptoms like those suffered by the patient.
Holistic medicine: This method looks holistically at the body, life force, soul and spirit. Care involves a holistic treatment with natural substances as well as conventional medical drugs.
Neural therapy: Neural therapy is based on the theory that trauma can produce long-standing disturbances in the electrochemical function of tissues. Treatment tries to affect the nervous system with injections of local anaesthetics.
Herbal medicine: Treatment is based on the principle of the healing powers of nature and avoids chemical additives.
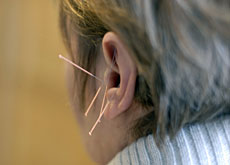
Traditional Chinese medicine: This method has been gradually developed ever since originating in China 3,000 years ago. It uses five methods for treatment: acupuncture, Chinese herbal medicine, massage, exercise and nutrition.
In 1999 the interior ministry ruled that five therapies – homeopathy, herbal medicine, neural therapy, traditional Chinese medicine and anthroposophic medicine – should be provisionally covered by basic health insurance. But this decision was reversed in 2005 amid rising national healthcare costs.
A national vote was held in May 2009 to decide if complementary medicine should be accommodated once again in the constitution.
The five treatments would be included on a list of paid health services. Diplomas for non-medical practitioners of alternative medicine would be recognised, there would be more collaboration between alternative and classical medicine and more research.
67% of people – 1.28 million – voted yes. 33% – 632,000 – voted no.
In December 2009, a federal commission on benefits recommended that complementary medicine did not met the requirements for reimbursement by insurance.
In January 2011 the interior ministry announced the start of a six-year trial period researching the efficacy of the therapies, and during which time their cost would be covered. This took into account current legislation which states that reimbursable therapies need to be meet criteria of “efficacy, cost-effectiveness and suitability”. The law also gives the interior ministry the right to decide whether to reimburse therapies under evaluation.
(With input from Christian Raaflaub and Andrea Clementi)

In compliance with the JTI standards
More: SWI swissinfo.ch certified by the Journalism Trust Initiative


You can find an overview of ongoing debates with our journalists here . Please join us!
If you want to start a conversation about a topic raised in this article or want to report factual errors, email us at english@swissinfo.ch.