‘You can’t test the virus away’

As Switzerland embarks on a major test offensive to combat a third Covid-19 wave, virologist Isabella Eckerle of Geneva University Hospitals – an outspoken testing advocate – cautions against treating it as a silver bullet.
Eckerle, who leads the Geneva Centre for Emerging Viral Diseases, has publicly championed more aggressive Covid testing throughout the pandemic. At times, she has also been a vocal critic of Switzerland’s approach to controlling the pandemic.
Last August, she warned that the country was “not well prepared” for a second wave and expressed concern that there was “no strategy” and “inconsistent testing”. Citing supply concerns, Swiss health authorities haven’t pushed for widespread, systematic testing across the country. Free tests have generally only been available to those with symptoms or those who know they may have been exposed to the virus.

More
Swiss plan free coronavirus tests for population
The government is now changing its tune as it waits on vaccine deliveries. On Friday, it confirmed a massive expansion of testing, with rapid tests available as of March 15 free of charge even for people without symptoms. Everyone will also receive five free self-tests a month when they become available.
Dr. Isabella Eckerle is the director of the Geneva Centre for Emerging Viral Disease, a joint institution between the University Hospitals of Geneva (HUG) and the Faculty of Medicine, University of Geneva. She was born in Germany and studied medicine at Heidelberg University. After a research trip in Africa, she became interested in infectious diseases and worked with German virologist Christian Drosten at the University of Bonn.
She specialises in viruses of zoonotic origin and has spent the last decade researching coronaviruses. Her lab led the development and validation of diagnostics for SARS-CoV-2 in Switzerland. She has also been investigating the role of children in the spread of the coronavirus.
SWI swissinfo.ch: Why did it take so long for Switzerland to pursue a more aggressive testing strategy?
Isabella Eckerle: I have the impression that in Switzerland there was a tendency to downplay the pandemic in many areas. This has affected testing to some extent because when many things are open, people are less motivated to get tested because they don’t want to face the consequences, such as going into quarantine.
We see this in our unit [at the hospital]. In the first wave, there was so much testing we could hardly manage. Our test positivity rate remains high now, but more people aren’t coming to the test centres. People have gotten tired of testing.
But Switzerland’s overall approach to testing changed a lot over the course of the pandemic. The criteria for testing changed and has varied across cantons, which has been very difficult.
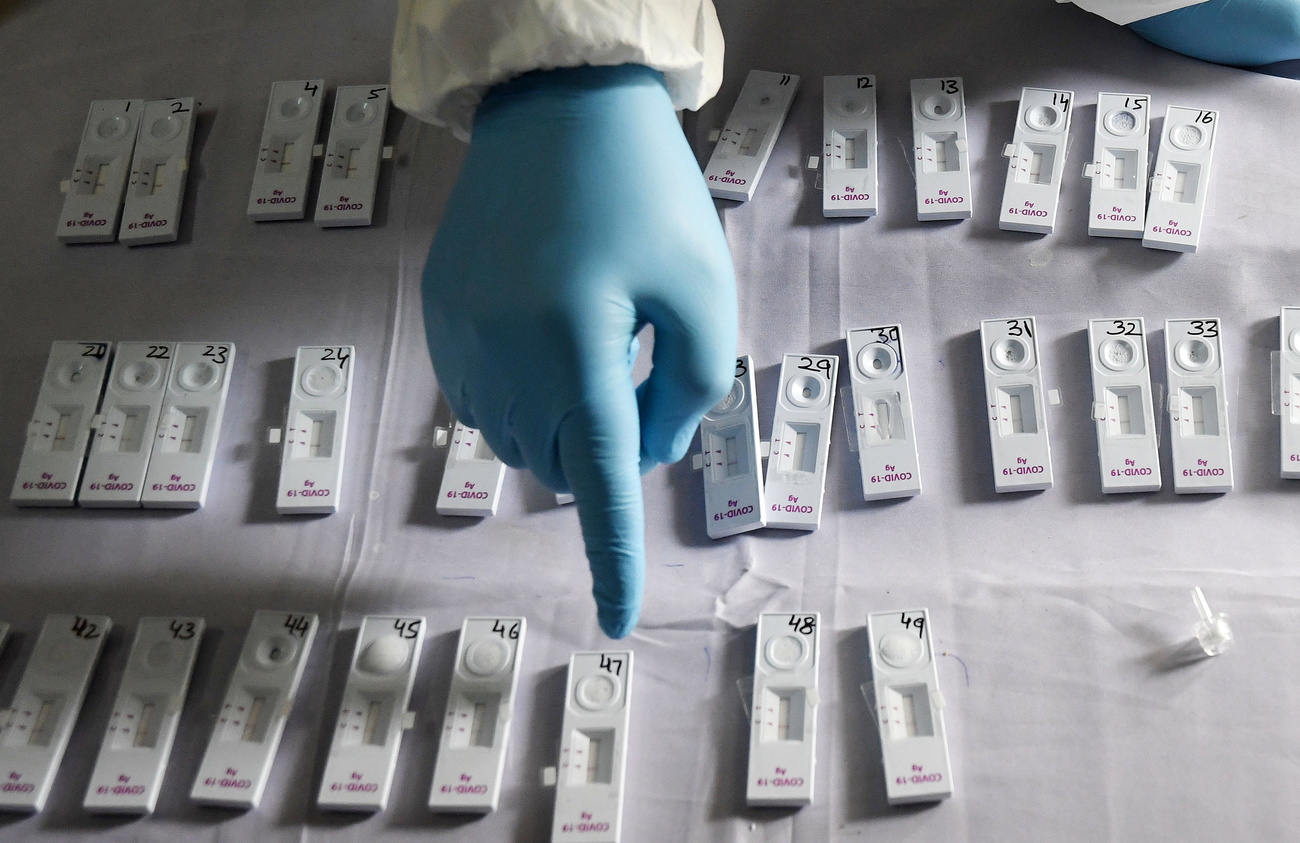
More
Rapid Covid-19 tests could offer a path back to normal
There were some things that Switzerland really did well. They were quick to make rapid antigen tests available already last year.
SWI: How much of an issue was the supply of tests?
I.E.: In the beginning, we weren’t equipped to run thousands of PCR tests a day. We had capacity for several hundred. When several manufacturers came out with automated systems, that helped but we still didn’t have enough reagents. This was solved over the summer.
There are now many tests on the market, so supply isn’t an issue. This will also improve with the introduction of home tests.
The difficulty is not only having the tests but rolling them out. This requires infrastructure such as test centres and training. There is also the question of what to do when you receive the results.
SWI: Do you think Switzerland’s announcement about free testing and at-home tests will help the country get a handle on the pandemic?
I.E.: I think this helps lower the threshold for testing, which is good. But the overall goals for managing the pandemic have to be clear. Do you want to keep hospitalisations down, or do you want to cut transmission? If you don’t have a good goal, you can’t adapt the strategy to it.
There are many areas where there should be more testing such as in schools and daycare centres. We know there are infections – and if we don’t find infections, we can’t break transmission.
There is no one solution though. We thought rapid tests were going to be a game-changer but nothing is a game-changer, even vaccines. We need to put everything together – protective measures, tests, vaccines. You can’t swap one measure for another. You need them all.
SWI: Do you think mass testing of an entire population in a region or city is effective?
I.E.: I haven’t seen convincing data that this changes a lot. It is a snapshot and you will put a lot of people in isolation while never bringing the transmission down to zero.
It really only makes sense if you can repeat it every few days, but I question the long-term strategy for mass testing in asymptomatic individuals.
SWI: Do you think that people should be able to show a negative test result to be able to do things such as go to restaurants or football games?
I.E.: You can’t test this virus away. You need to limit the spread with testing but you can’t replace the health protection measures with testing. This will not work. You don’t get a free pass because you did a rapid test.
Even if we have a lot of rapid tests, we can’t go back to normal because you will always miss people. The test is only a snapshot of that moment. It can be positive tomorrow. It is unrealistic to test yourself every day.
The key is to reduce the risk as much as possible, but testing can’t be used to open up everything. The question is how best to use these tests and how much risk we can accept. To me, it makes sense to test in schools because the benefits of keeping schools open are clear.
If a child tests positive in a school, why not have a mobile team go test the whole class? We know that kids can be asymptomatic so any positive cases can then get a PCR test to confirm.
SWI: You have done extensive research into transmission in children. What have we learned over the last year?
I.E.: We know that kids get infected and transmit the virus, but we don’t recognise it because they don’t get sick as often. They might not have respiratory problems but they may have other symptoms such as fatigue or stomach aches, which can be hard to pinpoint in kids.
In Geneva, the seroprevalence test [showing the share of the population that has been infected] after the first wave showed that children were much less likely to have been infected than adults. However, after the second wave, children above the age of six were almost as likely as adults to have been infected.
With regards to the emerging variants, studies in the UK show that a lot of children have gotten the virus but this may be because of the higher case rate in general. We also see from the UK that children can also have Long Covid.
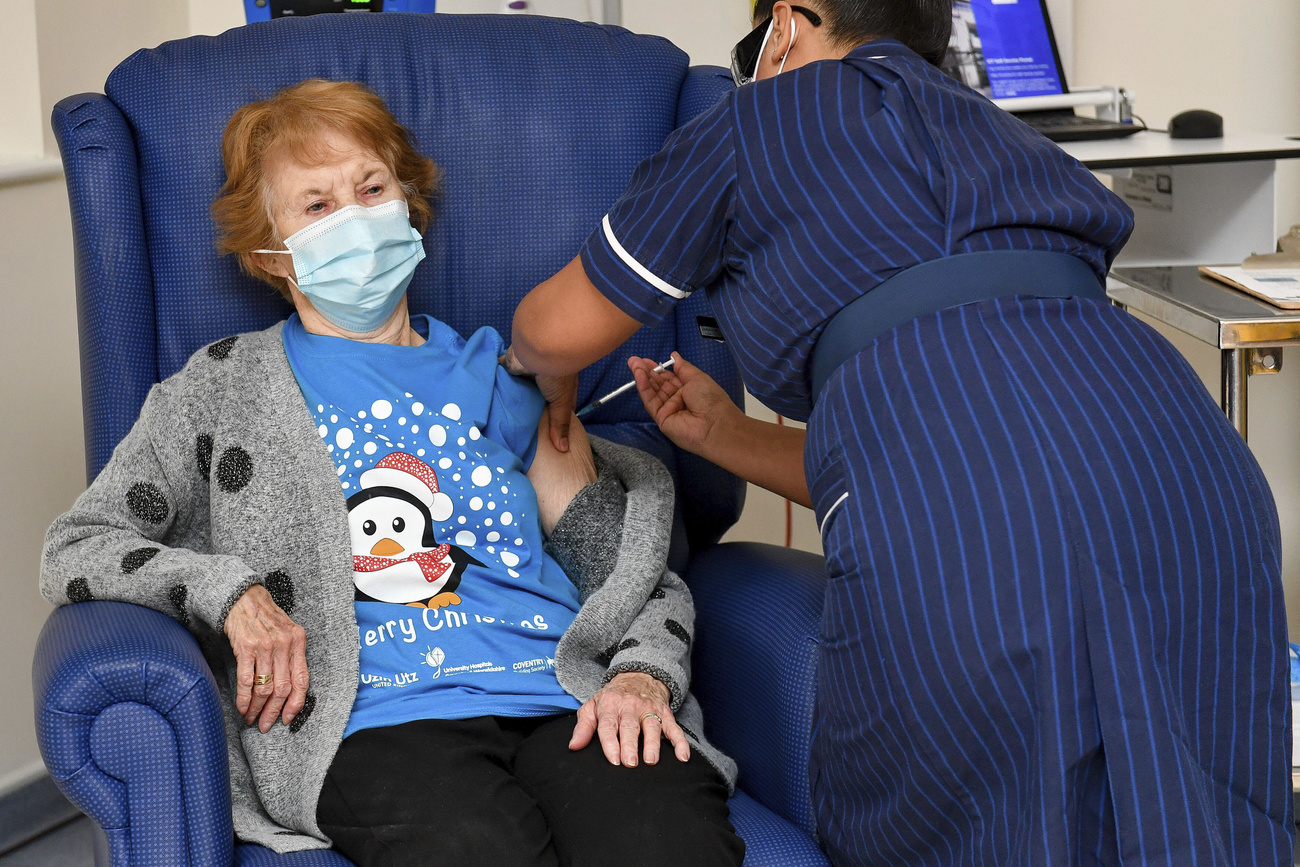
More
Covid-19 vaccine: Why we still have a long wait ahead
Switzerland has had an unusual stance on children. For example, young children aren’t wearing masks here whereas they are in many other countries.
There has been so much discussion about whether kids can get Covid, instead of focusing on easy measures to keep them safe such as smaller class sizes or masks.
SWI: What do you think we will take away from this pandemic?
I.E.: I hope that we focus on where these pandemics come from such as the destruction of habitats and how animals are used. We know there are many viruses out there that could follow the same route as this coronavirus. Wildlife trade, but also habitat loss, as well as mass farming of domestic animals are scenarios in which another spillover event of an animal virus becomes likely.
We need to focus on prevention. We knew that there was a risk of a virus similar to the first SARS but little was done about it. Like with the climate crisis, it will likely take many decades to see the payoff, but we need to focus on prevention now.
There has been huge innovation in vaccines – this is really a revolution in medicine – and so I do feel we will be more prepared to respond in the future.
On a societal level, the pandemic has made the inequalities that already existed more obvious. People with less well-paid jobs are at higher risk of diseases. We need things like paid sick leave on a global scale and social support.
SWI: What is the first thing you will do when this is all over?
I.E.: I will visit my family in Germany. I miss those frequent get-togethers with friends and family.
More

In compliance with the JTI standards
More: SWI swissinfo.ch certified by the Journalism Trust Initiative







Join the conversation!