Are robot-surgeons set to take over in Geneva?
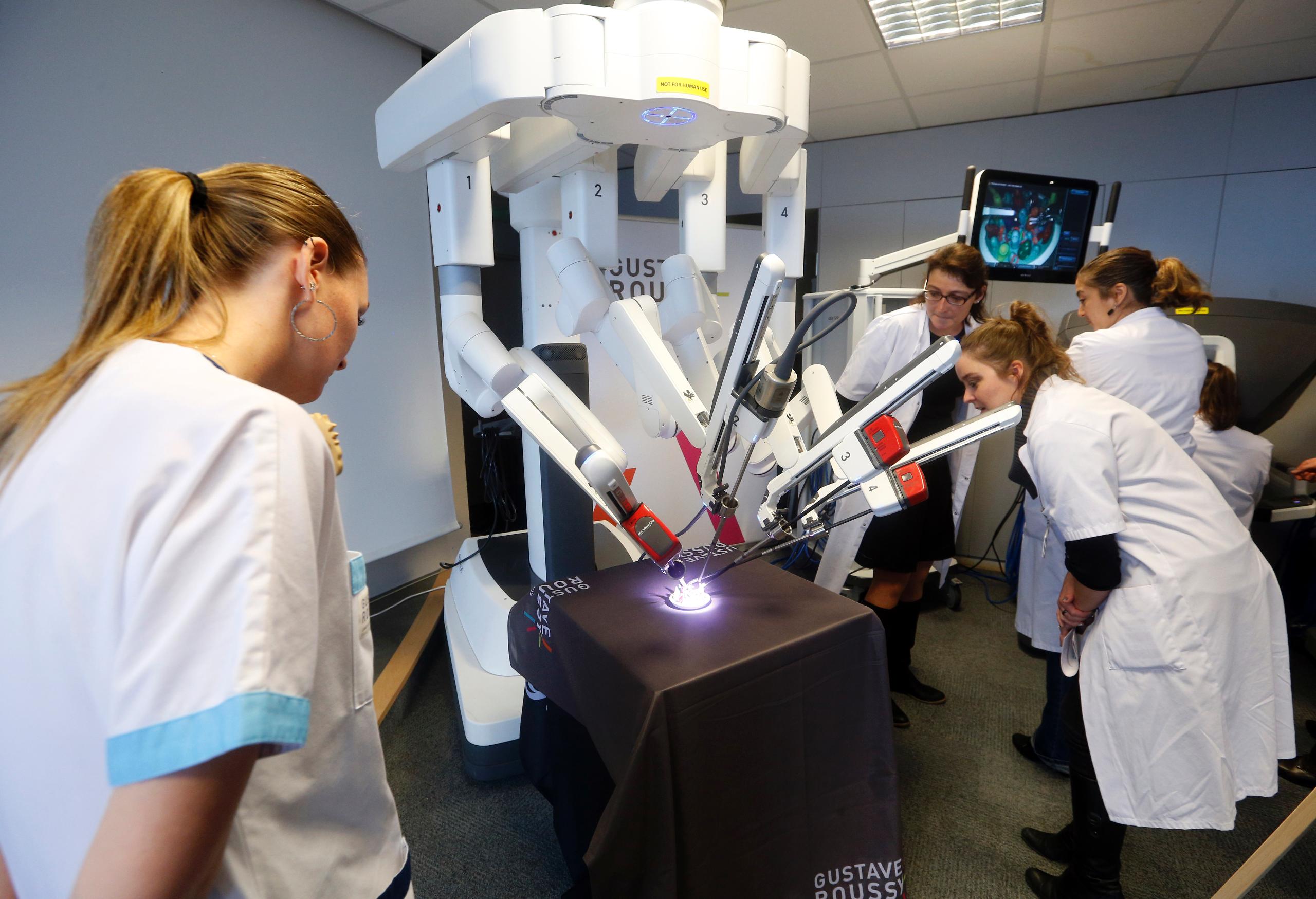
Geneva reportedly holds the world record for the highest concentration of Da Vinci robot-assisted surgical systems. Why is the canton so eager amid worries about high costs and safety compared with traditional surgery?
Geneva University Hospital (HUG)External link surgeon Philippe Morel is a medical robotics disciple.
“Robotic surgery is the future of surgery. There is no alternative,” enthuses HUG’s head of visceral surgery, who carried out the first gastric bypass operation in Switzerland with a Da Vinci Surgical System in 2010, the most common robotic surgery system.
Morel controls his “Octopus’s” instruments from the other side of the operating theatre, performing micro-accurate procedures on tissues deep within a patient’s body. The robotic system is used mainly for prostate operations, hysterectomies and other gynaecological procedures.
The public hospital and a number of private clinics in Geneva are big fans of robotic surgery. The HUG recently upgraded two of its three Da Vinci robots. The tiny canton of 400,000 residents has six Da Vinci systems – reportedly the most per inhabitant in the world.
For Morel and fellow surgeon Monika Hagen, the technical benefits far outweigh those of traditional surgery.
“It’s much easier. You are more in control. I really appreciate the freedom and manoeuvrability in tight spaces. The vision is superb with two cameras that create a true 3D image. That really helps to identify the structures that otherwise you might not be able to see. When you go back to normal surgery it’s painful,” says Hagen.
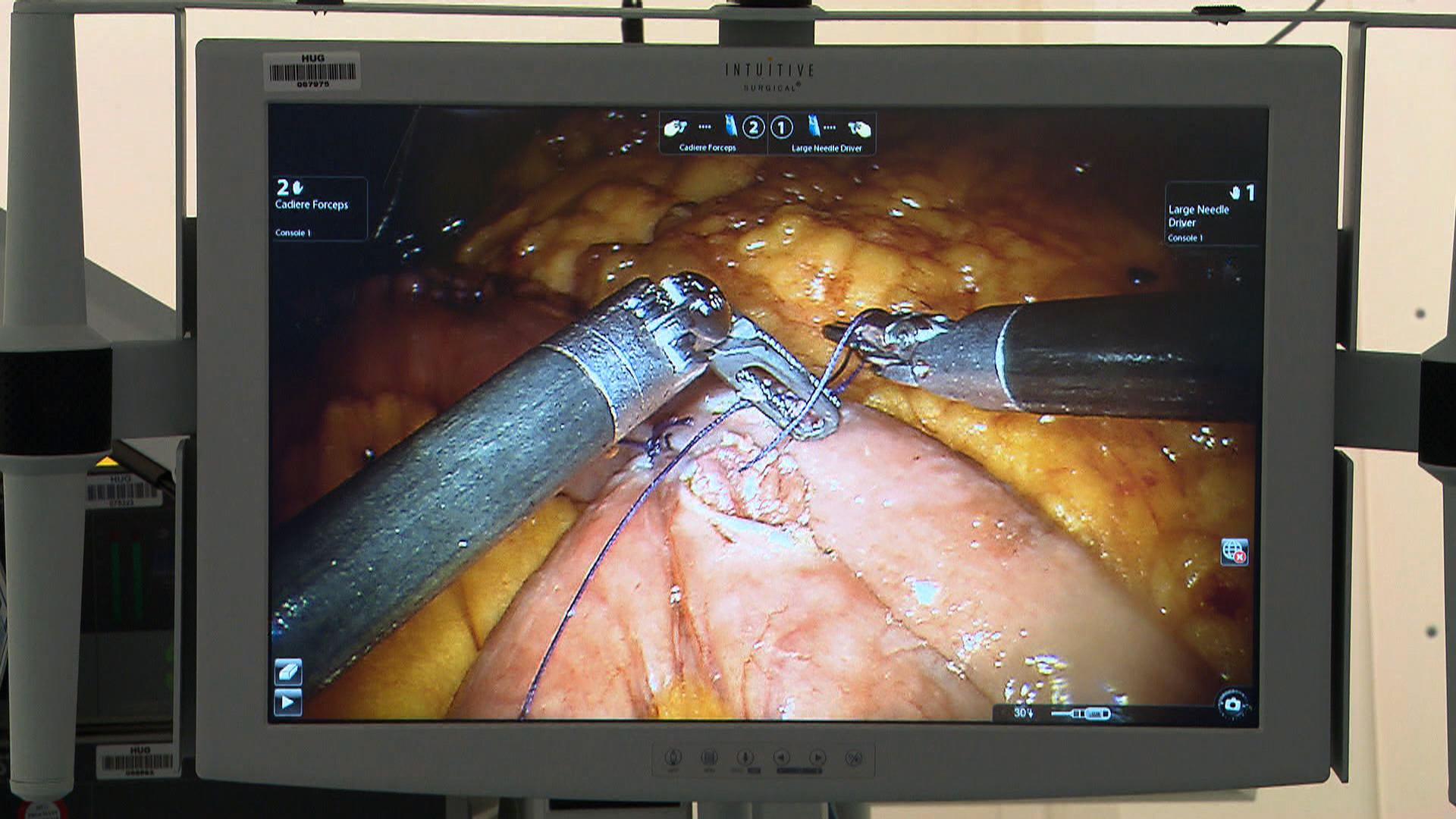
More
How robots improve surgery
Supporters argue that the far less invasive keyhole surgery reduces pain and blood loss for the patient, and minimises their time spent in hospital. Several members of the public who took part in a recent online forum on robotic surgery organised by Swiss public television, RTSExternal link, agreed.
Philippe had his prostate removed using robotic surgery in 2009: “I’ve had fewer after-effects and a fast recovery. This means fewer days in hospital and cost savings and greater comfort.”
For operations like removing prostates, discussion on the clinical benefits of the robot is ‘over’, said Hagen. For other operations, it was harder to say, she added.
In 2013, an extensive study by the American College of Obstetricians and Gynaecologists found that robotic surgery was not the best, or even the second best, option for hysterectomies, adding costs per procedure without any obvious benefit.
Spreading costs
One of the main problems with robotic surgery is the high cost. In a country like Switzerland, with ever-rising healthcare costs and insurance premiums, the growing number of expensive new machines raises questions.
A basic Da Vinci system costs about $1.5 million (CHF1.3 million) to buy. But hospitals also have to purchase additional instruments that are limited to a maximum of 10-20 uses, and the entire system comes with an annual maintenance fee.
For a Da Vinci to be financially viable, hospitals need to perform between 150 and 300 procedures annually for six years, Emmet Cole, a Texas-based robot expert, told the Financial Times.
The HUG has carried out 1,853 operations using the system since 2006. Hagen says surgeons there are fortunate, as no financial cap has been put on the use of robots for surgery or training. They have managed to spread the high up-front costs of their robots and make other cost savings thanks to numerous successful gastric bypass operations using the Da Vinci. In such cases the Da Vinci has resulted in fewer complications and post-operative costs and thus shorter stays in hospital, the HUG robot-surgeons claim.
Too many
But if the system is not managed properly, it can result in extra costs. So are those being passed onto health premiums? SantésuisseExternal link, an umbrella organisation for health insurers, says no.
“But there is a risk that hospitals equipped with these robots are practising more operations – without them being necessary – to make the new equipment profitable,” warns spokesman Christophe Kämpf.
There are currently 27 systems across Switzerland. Experienced HUG robotic surgeon Christophe Iselin says this is perhaps too many. He told the forum it made sense to cut the number in the French-speaking region.
“It’s clear that a certain number of robots in Switzerland are not being used to their full potential and that their under-use is contributing to the increase of medical costs,” he said.
100% safe?
Despite this rapid growth and claims the technology pushes the boundaries, the system is not infallible.
A March RTS documentaryExternal link highlighted the high number of incidents in the US – from minor to serious – in the past couple of years involving the Da Vinci system. In April 2014 the US Food and Drug Administration (FDA) said Intuitive Surgical,External link which produces the machine, had addressed violations, but the firm’s 2014 annual report still reported over 100 lawsuits.
Despite the worrying US statistics, Swissmedic, the Swiss Agency for Therapeutic Products,External link which oversees regulation, seems unperturbed.
Karoline Mathys, Swissmedic’s head of market surveillance, said there had only been a ‘handful of incidents’ involving Da Vinci robots since 2008.
In Geneva Morel and his colleagues insist they have never encountered any accidents with the same Da Vinci system and have always been properly informed by Intuitive.
Swissmedic relies solely on information from the firm and the “principle of responsibility”. Europe’s medical surveillance bodies, of which Switzerland is a member, have signed a confidentiality accord on the declaration of incidents. The user or manufacturer must highlight problems. Only corrective measures proposed by a firm are published.
“There is no evidence to show that we do not get enough information from the manufacturer or that there is a problem with Da Vinci robots,” Mathys told the RTS documentary.
Blame the surgeon
Rather than the robot, the main risk for patients, like always, is the surgeon, says Morel.
“75% of plane accidents are due to human error and not mechanical,” he said. “We know that we always have to work with the instruments in our field of vision. If an instrument leaves the field of vision you should never bring it back yourself as you do not feel the physical resistance and you can rip out vessels. This happened in the US.”
Improved safety comes essentially via better training, say the surgeons. HUG trainees complete a theoretical certification, followed by practical lab experience. But how do you know when you are ready as there is no exam or permit?
“Good question,” said Hagen. “Between 50-150 procedures…it depends.”
Training is another high but unavoidable investment cost. The robot is definitely here to stay, says Morel.
“In a few years there won’t be six Da Vinci in Geneva, there’ll be 15, in different disciplines. In 15-20 years, things will have totally changed. The patient will want to be sure that the surgeon is operating with a robot, with technical assistance increasing his precision,” he says.
And the surgeon will be much less present in the operating theatre, he adds.
“The surgeon will plan the operation beforehand and then carry it out virtually, registering their best operation, ensuring that the robot completes the recorded gestures and standing by in case there are any technical problems or need to adjust the technique,” he says.
Da Vinci robots, the most common machines, are produced by Intuitive Surgical, a US firm that currently holds the monopoly. Since the Food and Drug Administration (FDA) approved robotic surgery in 2000 in the US, about 2.5 million surgical operations using a robot have been performed there, according to the firm. About 3,200 machines are now operational, two-thirds in the US and over 500 in Europe. In Switzerland, there are 27. In 2014 Intuitive had revenues of $2.13 billion.
Google announced in March 2015 it was teaming up with Johnson & Johnson’s Ethicon subsidiary to build what the two hope are the ultimate platform for robotic surgery. It is thought Google will use its algorithm capabilities to analyse on-screen images and present the data in new ways for surgeons. A Johnson & Johnson spokesperson told wired.com this could include suggestions to surgeons on the best places to make incisions based on the individual patient’s medical history. Google says it will not be involved in making the systems that actually control the surgical instruments. Johnson & Johnson hopes the new system will be more cost-effective for hospitals in developing nations, and that it will have an interface that improves a surgeon’s access to information during a procedure.

In compliance with the JTI standards
More: SWI swissinfo.ch certified by the Journalism Trust Initiative


You can find an overview of ongoing debates with our journalists here . Please join us!
If you want to start a conversation about a topic raised in this article or want to report factual errors, email us at english@swissinfo.ch.