A day in the host of a malaria parasite

Ingenious, formidable and pernicious. These are just some of the words that are used to describe the deadliest of the malaria parasites, plasmodium falciparum.
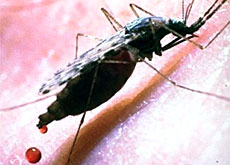
When an infected mosquito bites you, it injects saliva containing a form of the parasite into your bloodstream.
Within 30 minutes – too short a time for your body to muster an effective defence – these threadlike structures, called sporozoites, penetrate your liver cells. Here they remain for a week or so, multiplying furiously.
Just before the body’s killer T cells have time to react, the parasites break out of the liver.
Out of control
By now, they are no longer sporozoites but a rounder, more compact form known as merozoites. For every one of the former, there are up to 40,000 of the latter.
Within minutes they have invaded red blood cells where, protected from the immune system, their numbers increase once more.
Every 48 hours the cells rupture, the parasites burst out and colonize yet more red blood cells, beginning the cycle again.
Meanwhile, some of the parasites in red blood cells develop into sexually mature gametocytes, which are sucked up by mosquitoes when they bite an infected person.
When a drop in temperature tells them they are in the mosquito’s gut, they emerge from the blood cells.
In a process that depends on the outside temperature but takes at least eight to ten days, they reproduce inside the mosquito, forming a sac containing thousands of new sporozoites.
The sac ruptures and the sporozoites travel to the mosquito’s salivary gland ready to enter another victim when the mosquito takes its next blood meal.
Fever
When the parasites are in your liver, you do not feel sick. It is when the red blood cells burst that toxins are released into the bloodstream.
At this stage, some nine to 14 days after the initial mosquito bite, a person feels the first signs of infection – high fever, chills and profuse sweating. These symptoms come in waves each time parasites break free.
Red blood cells carry oxygen from the lungs throughout the body. When they rupture, they cripple the body’s ability to transport oxygen. If too many are damaged, a person becomes anaemic.
Chronic anaemia affects immunity to other diseases and many children in Africa die of diarrhoea or pneumonia, measles or the common cold, which they would otherwise be able to fight off.
In other cases, death is due to infected red blood cells blocking the narrow blood vessels in an organ of the body and starving it of oxygen. If blood vessels of the brain are affected, the condition is called cerebral malaria and produces convulsions and coma.
In pregnant women, reduced oxygen and nutrient supply to the developing foetus results in low birth-weight babies, stillbirths and miscarriages.
If left untreated, falciparum will kill up to a third of the people it infects. If you do not die and you do not get antimalarial treatment, you can rid yourself of the disease after a few years. In endemic areas, however, people are constantly reinfected with parasites.
Genetic disorder
Malaria is such an ancient and virulent disease that it has affected human evolution.
In endemic areas, people’s chances of survival increase if they are carriers of the genetic disorder, sickle cell anaemia.
This lethal disease is caused by defective haemoglobin – the protein inside red blood cells that carries oxygen.
Children who inherit a copy of the mutant gene from each parent usually die at an early age.
Children who inherit a copy from only one parent do not develop the disease but have sickle cell trait. In other words they are carriers of this genetic mutation.
Sickle cell trait protects young children from the effects of severe malaria but the price that parents pay is the risk that their offspring will inherit both defective haemoglobin with fatal consequences.
If both parents are carriers, there is a 25 per chance their child will have sickle cell anaemia, a 50 per cent chance of being a carrier and a 25 per cent chance of being unaffected.
The disease is particularly common in tropical Africa. A related disorder, thalassaemia, is prevalent around the Mediterranean. Its occurrence to this day is testimony to the former severity of malaria in southern Europe and the Middle East.
swissinfo, Vincent Landon
Malaria is transmitted through the bite of a female anopheles mosquito.
Symptoms – fever, shivering, headache and vomiting – appear about nine to 14 days after an infectious bite.
Malaria is a curable disease if promptly diagnosed and treated.
If drugs are unavailable, the infection can rapidly become life threatening and children often die less than 72 hours after developing symptoms.
Malaria kills by infecting and destroying red blood cells (anaemia).
It can clog the vessels carrying blood to the brain (cerebral malaria) or other vital organs.

In compliance with the JTI standards
More: SWI swissinfo.ch certified by the Journalism Trust Initiative
You can find an overview of ongoing debates with our journalists here. Please join us!
If you want to start a conversation about a topic raised in this article or want to report factual errors, email us at english@swissinfo.ch.