Coronavirus: A turning point for telehealth in Switzerland

The Covid-19 pandemic has given a new impetus to telehealth, with lockdown leading to an increase in remote medical consultations. Patients are now returning to doctors’ practices, but the digitisation of health has become standard – even if not all are persuaded of the benefits.
Booking a doctor’s appointment or receiving test results online has been commonplace for years. Remote medical consultations, however, were still a peripheral phenomenon. Patients and doctors were sceptical: How do we build a rapport? How do we guarantee the privacy of data? How do we reach the right diagnosis?
So many questions that remained unanswered for a long time…
Coronavirus – an innovation booster
In March the coronavirus crisis changed all of this. Given the risks, remote consultations became the de facto norm for doctors, says Arthur Germain, the director and founder of the website OneDoc, which specialises in arranging doctors’ appointments online.
“We have wanted to develop a video consultation tool for a long time, but we always got the impression doctors weren’t ready for it, so we shelved the project,” Germain says. “Covid-19 was a massive impetus however: our developers worked hard for a week to build a coded video platform.”
With the virus, demand exploded. “Within two months, it increased tenfold,” Germain says. He has registered almost 2,000 specialists on his website, 500 of them for this new service.

Until the end of the pandemic, the service is free for all those in the medical professions who register. The Geneva start-up hopes to convince doctors of its method, and aims to be more efficient than the telephone and more secure than other video services such as Facetime, Skype or Zoom.
“If the quality is good, then video is a real bonus,” says Eric Bec, a general practitioner and head of the Teomera health centre. “At the beginning of the crisis, I had patients on the telephone, but it was complicated to give a diagnosis without seeing them. So I used Whatsapp at first, then OneDoc, to decide who could stay at home and who needed to come to the centre for a consultation.”
Other doctors are more negative about their experiences with remote consultations. “We had to fall back on them when necessary,” says Mouncef Berrada, the leader of the medical and surgical centre in Cornavin. “But we won’t introduce them permanently. You can’t solely rely on what a patient says without examining him physically. A video is not enough.”
Medicine 2.0
At the Geneva University clinic, Sanae Mazouri, a doctor, didn’t wait for the coronavirus to clear the path for telehealth. She had already launched the project HUG@home in May 2019: a platform with a chat, audio- or video-calling system connecting the doctors at the hospital with caregivers at the Spitex nursing home.
“Our goal was to encourage patients to stay home to regulate the flow of emergency cases, and to save time and reduce the costs of transfers back to the hospital,” says Mazouri. “We tested our application for six months with patients who had been discharged from the university hospital and were being cared for at the Spitex. The experiment was conclusive – in nine out of ten cases, we could avoid a transfer back to the hospital.”
Given the encouraging results, she had the idea of extending the service from 2021 to patients undergoing treatment for chronic illnesses. And she added a remote consulting service that is directly accessible for all patients after triage to assess their care needs.
The pandemic accelerated the process… “In order to react to the health emergency and avoid overwhelming the hospital, we spent two days working to offer all the doctors in the city a new version of our application which was renamed Docteur@home,” Mazouri says. Since then, the service has gained more than 900 professional users at the university hospital and almost 400 doctors in the canton of Geneva.
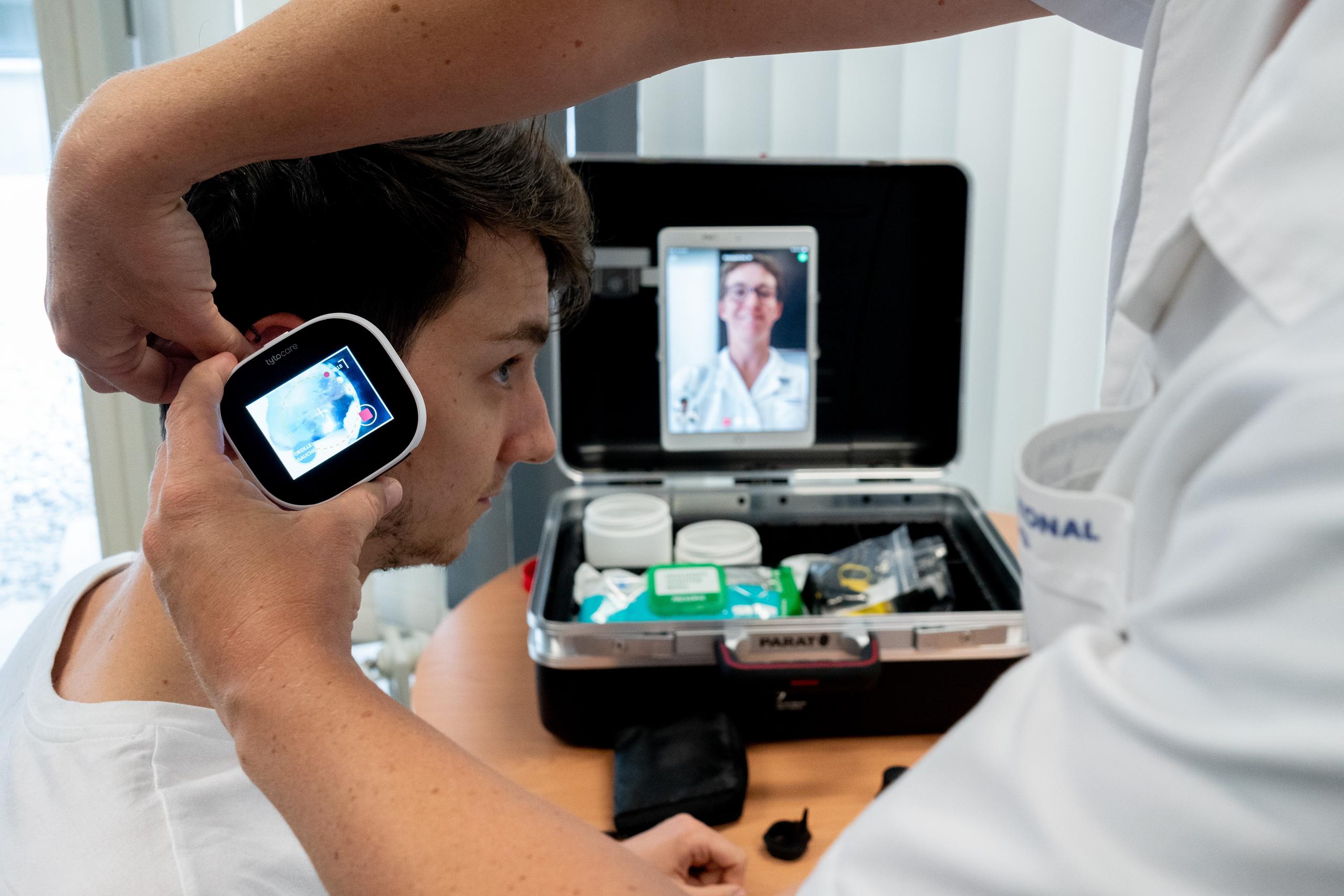
The Fribourg hospital is also laying emphasis on telehealth. In April, medical director Ronald Vonlanthen presented a project supported by the canton: a suitcase with medical equipment to allow the remote treatment of patients.
“Coronavirus revealed two big risks to our health system: the risk that hospitals could be overwhelmed and the isolation of patients who are deemed at-risk. With our suitcase, we bring the medical treatment they need to them at home,” says Vonlanthen. “We give the patients treatment in advance to limit the number of transfers to the hospital resulting from complications.”
During the crisis, trainee nurses were deployed as mediators to support patients during the remote consultation. But this ambitious project costs CHF50,000 and Vonlanthen is still looking for investors to develop it for the long term.
Over-digitising?
The digitisation of health is not met with enthusiasm everywhere by medical staff. Most practising doctors have taken up physical consultations in their practices again.
“Telehealth can give you an idea of the patient’s symptoms,” says Gilbert Geinoz, a GP in Geneva. “But face-to-face health is in my view a better way to reach a diagnosis and above all, appropriate treatment.”
Many doctors, nursing staff and therapists even worry about their professional future and complain about “over-digitisation” in health. “This is not my idea of medicine,” Berrada says. They all emphasise the importance of human contact between doctors and patients.
This is particularly important in the area of mental health, where telehealth has made some inroads in recent years, especially in the United States. “Analysing the non-verbal body language is a matter of fundamental importance in our profession,” says Pierre-André Mayor, a psychiatrist and psychotherapist in Geneva.
“Remote consulting has allowed me to maintain a therapeutic connection to my patients during the crisis, but in my view it worked primarily because I had already built a rapport with them.”
It’s too early to say if the coronavirus has delivered a death blow for traditional medicine. According to Arthur Germain, however, the health professions will inevitably develop further towards digitisation. “Medical staff will have to adapt in order to meet patients’ new expectations,” he says.
Ronald Vonlanthen remains optimistic about the human contact inherent to medicine.
“New technologies and artificial intelligence will change the way medicine is practised and new medical careers will open up. But in order to make a diagnosis, we will always need a human brain behind the machines,” he says.

In compliance with the JTI standards
More: SWI swissinfo.ch certified by the Journalism Trust Initiative


You can find an overview of ongoing debates with our journalists here . Please join us!
If you want to start a conversation about a topic raised in this article or want to report factual errors, email us at english@swissinfo.ch.