
Telemedicine defined by hope and doubts
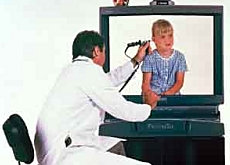
As telemedicine becomes more and more widespread, Swiss researchers warn the risks and benefits of this type of healthcare must be properly evaluated.
Although it could give better access to medical treatment, telemedicine also threatens to end the traditional patient-doctor relationship and violate medical confidentiality.
Telemedicine has been defined as using telecommunications technology to provide medical information and services. This extends from a simple phone call between a doctor and his patient to remote surgery using robotic equipment.
“At the moment it is mostly sharing knowledge, such as consulting a patient from a distance,” said Robert Sader, deputy head of the centre for multidisciplinary research in cranio-maxillofacial surgery at the Basel University hospital.
“But it also involves sending data [using telecommunications technology] to another location with the right competences for analysis and getting the results back.”
In Switzerland, the use of advanced remote technology in medical services is still in the development stage. Individuals or institutions have initiated most current projects as much out of practical need as out of scientific interest.
Cantons Geneva – where an electronic patient file has been developed – and Ticino – with its patient card and electronic network – host the most advanced telemedicine projects in the country, boosted by local government support.
Remote surgery
Researchers working for the Swiss Centre for Technology Assessment (TA-Swiss) said in a recent report that while the country has an optimal communications network for telemedicine, progress is being hampered by a lack of coordination.
Among other problems cited are the difficulty of making the best use of the knowledge gained by doctors and the risk of developing more infrastructure than necessary.
For Sader, who is also a professor at the Wolfgang-Goethe University in Frankfurt, telemedicine is already a tool he uses regularly, relying on videoconferencing to discuss cases with colleagues elsewhere.
He uses telemedical technology too when planning an operation.
“In surgery, every operation is unique,” he told swissinfo. “But with telemedical applications, we can share knowledge, meaning we can repeat the same operations many times with better results.”
Perhaps the best-know telemedical application is robotic surgery involving a doctor in one location and a patient in another. While it is spectacular, Sader is not convinced that this is necessarily the progress some specialists claim.
“Remote surgery looks nice on paper, but it cannot deal with complications at the moment,” he said. “If you have a problem during an operation, you have to be able to manage it remotely, and that’s not possible.”
Remote surgery also highlights another problem with telemedicine: the risk of undermining the relationship between a doctor and their patient.
“Personal contact with a patient is very important and we have to make sure we don’t lose it,” added Sader. “It’s very hard to establish trust between a patient and a doctor remotely.”
The surgeon says that the best solution is for a patient to be with a personal physician when consulting a specialist via a telemedical application. The specialist supplies missing medical expertise while the doctor provides the personal touch.
Cost
Another factor that intervenes in the use of telemedicine is cost. The TA-Swiss report claims that extensive use of telemedical applications could translate into savings for the healthcare system, and also make it more attractive for foreign patients.
Sader says this makes sense.
“The costs of buying medical knowledge will go down,” he told swissinfo. “For some types of treatment, telemedical applications will allow us to cut costs, and that’s good for society.”
And he plays down fears that telemedicine will be the preserve of the wealthy.
“The problem at the moment is that if someone can afford it, that person will travel to wherever necessary to get the best treatment,” he added. “Telemedical applications can make this all cheaper, making it more affordable for more patients.”
But with more extensive use of telemedicine on the cards in the longer term, privacy and confidentiality issues will also be raised. The TA-Swiss researchers say security will be at a premium with electronic transmission of patient data on the rise.
Sader reckons this is nothing new. “Confidentiality problems can start simply with a telephone call since there are no guarantees someone isn’t listening in,” he said.
He added that to ensure the best possible security, it wouldn’t be up to the doctor to choose what must remain confidential.
“With telemedicine applications, we have to decide what kind of information needs to be secure,” he admitted. “The patient is the best person to make clear what must remain completely confidential.”
swissinfo, Scott Capper
The Geneva «e-toile» project focuses on computer-based patient files.
Treatment data can be stored on these files, and called up.
The idea is to connect all healthcare institutions via a medical information network, at the heart of which is the electronic patient dossier.
Strict security is imposed on the transmission of patient data.
To give patients some control, they can use an access card to specify who is authorised to access their data on file, and to what extent.

In compliance with the JTI standards
More: SWI swissinfo.ch certified by the Journalism Trust Initiative



























You can find an overview of ongoing debates with our journalists here . Please join us!
If you want to start a conversation about a topic raised in this article or want to report factual errors, email us at english@swissinfo.ch.