Syphilis cases on the rise
In honour of World Aids Day, Switzerland has unveiled a prevention programme for 2011-2017; it aims to fight HIV as well as other sexually transmitted infections.
The inclusion of STIs like chlamydia, gonorrhoea and syphilis is new. Recent statistics show the need to address these illnesses in addition to HIV and Aids.
For example, the year 2010 has seen a higher incidence of syphilis in Switzerland than previous years. As of November 29, the Federal Health Office had recorded 1,026 cases of syphilis – considerably more than in 2009 (716 cases) and 2008 (665).
“What we see in our daily practice is a mirror of what is going on outside the world of HIV-positive patients. What we have seen during the last 10 years is a massive increase in syphilis, which probably means that there is more unprotected sex going on,” according to Hansjakob Furrer, a doctor at Bern University’s infectious diseases clinic at the Inselspital hospital.
As Furrer explained, people were more careful in the 1990s, when most knew of somebody who had died or was dying of Aids. This helped lead to a decline of syphilis in the 1990s.
Yet people became more careless after 2000 – including the authorities. Between 2000 and 2006, Swiss doctors were no longer required to report suspected cases of syphilis.
“It is possible that, having suspended surveillance, that some transmission that was going on – and was going to cause an outbreak – didn’t get detected,” noted Nicola Low, epidemiologist at Bern University’s institute for social and preventive medicine.
She pointed out that syphilis incidence had gone up in many countries over recent years and that there were outbreaks of syphilis from time to time.
“It’s not clear whether that’s what’s happening in Switzerland at the moment,” Low told swissinfo.ch, adding that it was difficult to compare Switzerland with other countries; Swiss figures include suspected cases, while other nations only count the confirmed cases.
Transmission
The majority of those who contract syphilis are male. In 2009, it was more than 80 per cent.
“Syphilis transmission remains uncommon in the heterosexual community. Most syphilis transmission takes place between men who have sex with men, so that’s a group that really has to be careful,” Low said.
While a condom is generally considered the best protection against STIs, many find the method hard to adopt – at least for oral sex. And although the risk of HIV infection is very low if there is no ejaculation and no blood, the risk of contracting syphilis is very real.
“Syphilis is transmitted quite easily by oral sex, unlike HIV – which is difficult to transmit in that way. So if we see patients who have new syphilis and we ask them if they protect themselves, they often say ‘yes – always’. But then we find out that they had unprotected oral sex,” Furrer told swissinfo.ch.
Diagnosis
What can be difficult is knowing whether you’ve got syphilis to begin with. The primary lesions are typically painless and might even go unnoticed, depending on their location.
“If you see the primary lesion of syphilis, it’s rather easy to diagnose, but this is an ulcer that is not painful – so many patients don’t realise that it could be syphilis – especially when it goes away without treatment,” Furrer said.
It is not until the secondary stage that skin eruptions break out; the tertiary stage can affect virtually every organ. However, between the stages, there may be very few symptoms or none at all. (See box.)
“Doctors need to keep syphilis in mind when they see possible symptoms or get aware of risky behaviour, because it’s easy to identify it through a blood test,” Furrer said.
The cure
It is also fairly easy to cure syphilis, either with injections of penicillin or a three-week course of antibiotics, according to Low.
“Untreated syphilis has many risks, including severe neurological damage and heart disease, and pregnant women can pass it on to their babies,” Low said. Worldwide, congenital syphilis causes about half a million foetal deaths a year.
As Furrer added, “The risk of getting infected with HIV is higher if you or your partner has active syphilis – for example, sores in the genital region”.
In any event, keeping partners in mind is essential, according to Low.
“The important thing with any STI is to remember that it has to have come from somewhere, and you have to make sure that your sexual partner or partners also get treated.”
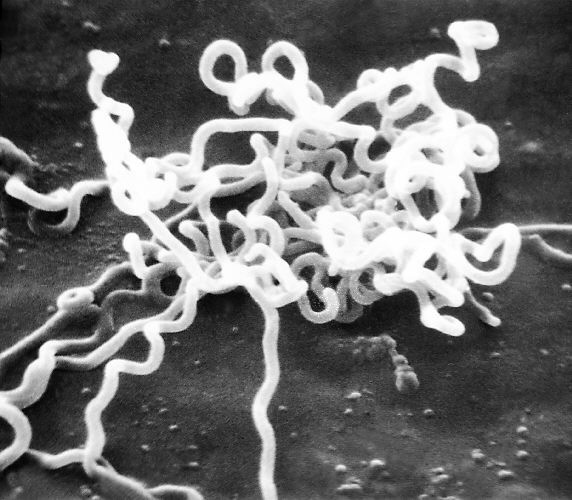
Pathogen and transmission
Syphilis is a chronic sexually transmitted disease. The pathogen is the Treponema pallidum bacteria. Syphilis is transmitted mainly through sexual acts via mucous membrane contact. The disease can be transmitted during pregnancy and to the child at birth. In stages 1 and 2, syphilis is highly contagious.
Stage 1: Syphilis presents itself (10 days to 3 months after infection) with painless lesions and lymph node swelling. The boils disappear after 4-6 weeks without treatment.
Stage 2: Flu-like symptoms, lymph node enlargement, often with a skin rash. These symptoms also disappear without treatment after a few weeks or within a year. Skin lesions can also occur in the following years.
Stage 3: Destruction of the central nervous system, organs, muscles, skin. Neurological problems leading to paralysis and dementia.
Prevention via “safer-sex”
1. Penetration with a condom
2. No semen or blood in your mouth
The cure
Syphilis has been curable since the discovery of penicillin. This resulted in a significant decline of the disease in the 20th century. Since the 1990s, a worldwide increase has been observed again. In Switzerland, around 350 people are infected with syphilis every year (12 million worldwide).

In compliance with the JTI standards
More: SWI swissinfo.ch certified by the Journalism Trust Initiative





You can find an overview of ongoing debates with our journalists here . Please join us!
If you want to start a conversation about a topic raised in this article or want to report factual errors, email us at english@swissinfo.ch.