Skin graft progress gives hope to burn victims
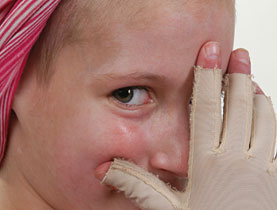
Swiss scientists and doctors are hoping to make skin grafts more cosmetically pleasing with the development of a skin substitute that is as close to human skin as possible.
They work inside the Paediatric Burn Centre at Zurich University Children Hospital – the first of its kind in Switzerland which treats around 400 young burns victims each year.
The suffering of young patients at the centre is often great as some have more than 50 per cent burns.
“Fifty to 60 per cent of our patients are aged between zero and three years old and usually have a scald injury from hot water,” said Clemens Schiestl, the centre’s director.
“Forty per cent are older children, usually boys, who have played with fire or fireworks.”
Another scenario is when adults use kerosene to speed up BBQs or fondues and children bear the brunt of the flare up.
“It’s a hard situation for a father who uses kerosene and causes 60 per cent burns in his child,” Schiestl told swissinfo.
Such cases need prompt medical action in the ward. First Schiestl and his team have to make sure that the body’s shock reaction does not cause the blood circulation to collapse.
The children are given a lot of fluid at this stage – a child’s body weight might rise from its usual 20 kg to 40 kg – but it allows doctors to save his or her life.
Once a child is stable, the burned skin, which can release toxic substances into the body, has to be removed. In high percentage burns this causes a large wound – and it is essential to stop it from becoming infected.
Skin grafts today
This is where skin grafts come in. For this the patient’s own skin is used, mostly from the scalp.
It can be a long process, with an operation every second day for up to five weeks. “It’s a very hard time for the patient,” explained Schiestl.
The skin gradually becomes stable and the patient has to wear pressure garments. As the grafts do not grow with the youngster, joint areas may need to be redone.
Patients with 50-60 per cent burns can expect to return home after three to four months. Here the centre helps the parents – staff check if the bathroom is suitable and help with the child’s return to school.
The skin, red and swollen, gradually calms and regains some of its original colour.
The rehabilitation programme is usually stopped after a year, but the centre’s philosophy is to follow the child’s progress into adulthood.
“We look out for all the problems, when a child starts school, when they first fall in love as an adolescent,” said Schiestl.
The teenage years can be difficult for disfigured children – burns are often on the face and arms. However, around 90 per cent of young burns victims go on to lead a normal life.
Work of tomorrow
Schiestl says that operations always result in scarring.
“The only hope of improving the situation are laboratories like Dr Reichmann’s, which are working on having, in around ten years’ time, skin that looks like normal skin after it is grafted and not like a scar,” said the doctor.
Ernst Reichmann is a cell biologist and skin engineer, whose pioneering Zurich laboratory – one of only a few around the world – is working on advanced skin grafts. Founded in 2001 it is a unit of the children’s hospital and works closely with the burns centre.
“We would like to produce full thickness skin substitutes that surgeons can apply to the patient in only one surgical intervention, which is not possible nowadays,” Reichmann told swissinfo.
At present, doctors use a bovine collagen that is covered by a silicon membrane for severe burns. Over time the collagen, which acts as the artificial dermis or skin middle layer, is replaced by the patient’s tissue.
The silicone membrane, the epidermis or outer skin layer, then has to be removed and replaced with the patient’s skin.
“In some cases surgeons have to mesh the skin – cut holes in it – and stretch it to get more tissue… and in many cases cosmetically this is not at all satisfying,” explained Reichmann.
The team is working on developing a graft that contains both the dermis and epidermis made from the patient’s own cells.
Cells and blood vessels
These are taken from a small biopsy and expanded in culture in the laboratory. A problem is that during this process all of the skin’s self-renewing cells are lost. This means that grafts would “melt away” because there are no cells to generate new tissue.
The team therefore has to make sure there are enough of these cells in the graft before it goes to the patient.
A second problem is that the dermal part of the graft is not vascularised – it has no blood vessels to supply it with the nutrients and oxygen it needs. This is needed for tissue survival.
Scientists have to pre-vascularise the graft in the lab so that it can connect quickly to the patient’s bloodstream.
So far they have created a sample of about three centimetres in diameter as a “biologically very active hydrogel”. The aim is to produce ten to 15 centimetres for surgical use.
It is very detailed work. “Our aim is also to give skin back its colour because currently during skin replacement the colour cells are lost and the skin is white,” added Reichmann.
The research is carried out in close collaboration with the medics. At first, admit Schiestl and Reichmann, the two separate disciplines had to “learn to speak each other’s language”. But now collaboration is successful.
“It may be a while before the new skin is ready,” Schiestl said. “But I’m sure that every day we are working on the ward and in the lab we are coming a little bit closer to this aim.”
swissinfo, Isobel Leybold-Johnson in Zurich
The skin is the body’s largest organ, covering the entire outside of the body.
It consists of three layers of tissue: the epidermis, an outermost layer that contains the primary protective structure, the stratum corneum; the dermis, a fibrous layer that supports and strengthens the epidermis; and the subcutis, a subcutaneous layer of fat beneath the dermis that supplies nutrients to the other two layers and that cushions and insulates the body.
Human skin is enormously well supplied with blood vessels; it is permeated with a tangled, though apparently orderly, mass of arteries, veins, and capillaries.
In a first-degree burn, only the epidermis is affected. These injuries are characterised by redness and pain; there are no blisters, and edema (swelling due to the accumulation of fluids) in the wounded tissue is minimal. Sunburn is an example of a first-degree burn.
The damage in a second-degree burn is deeper as it extends through the entire epidermis and part of the dermis. These injuries are characterized by redness and blisters and often considerable swelling. Both first- and second-degree burns can be very painful.
Third-degree burns destroy the entire thickness of the skin. The surface of the wound is leathery and may be brown, tan, black, white, or red. There is no pain, because the pain receptors have been obliterated along with the rest of the dermis. Blood vessels, sweat glands, sebaceous glands, and hair follicles are all destroyed. These burns are classified as medical emergencies.
Source: Britannica online encyclopaedia

In compliance with the JTI standards
More: SWI swissinfo.ch certified by the Journalism Trust Initiative


You can find an overview of ongoing debates with our journalists here. Please join us!
If you want to start a conversation about a topic raised in this article or want to report factual errors, email us at english@swissinfo.ch.