How an app is helping women self-diagnose perinatal depression

After her own experience with postpartum depression, a former pharma executive realized that the condition is drastically undertreated in Switzerland and around the world. So she quit her job and went on a journey to try to find a unique solution.
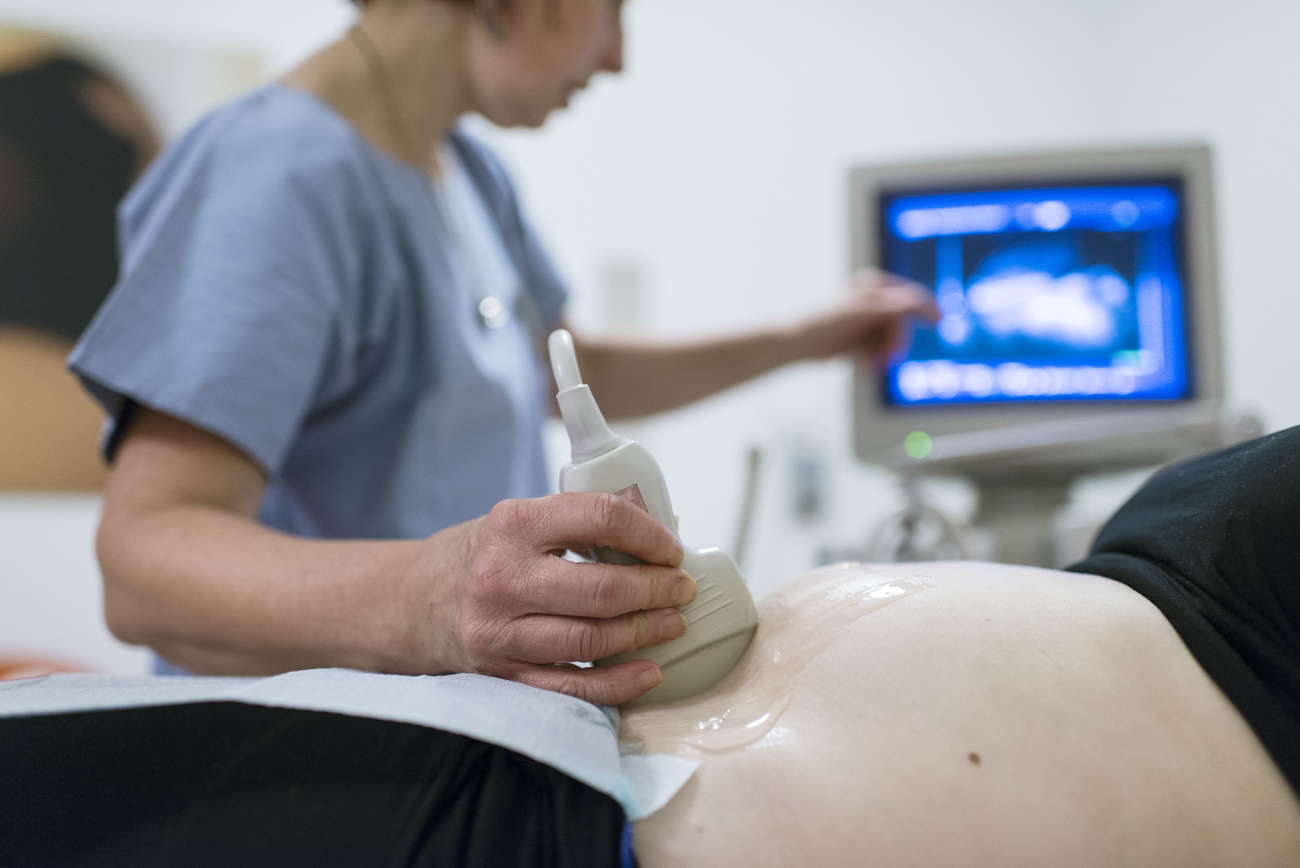
“After the birth of my twins in the United States, out of nowhere, I was totally overwhelmed by severe postpartum depression (PPD). Like many new moms, I fell through the cracks with the pressure to be a ‘perfect mother’ and didn’t seek treatment,” says Sonali Mohanty Quantius, a former pharmaceutical executive. She is the founder of HaplomindExternal link, which is creating a digital platform for screening, management and treatment for perinatal depression.
PPD manifests itself in severe mood swings, crying spells, insomnia, intense irritability and anger after the birth of a child. Only around 12% of the 50 million women diagnosed with the condition worldwide every year receive treatment. Quantius was plagued by severe PPD for four years and finally overcame the depressive disorder herself through long-distance running training. She realised that she had never received screening or treatment for the condition despite living in the United States, which has clear screening recommendations, and falling into a risk group as the mother of multiple births.
In England, the Edinburgh Postnatal Depression Scale (EPDS) is used consistently by different professionals, twice to three times in the first 6-8 months after childbirth. Similarly, routine screening using the Edinburgh Postnatal Depression Scale is recommended in pregnant women in the United States and Australia. However, the premise of widespread use of EPDS for screening is that professionals are trained in its use, and clear criteria and guidelines for the interpretation of the screening test results and possible interventions are available.
Perinatal depression includes depression that begins during pregnancy (called prenatal depression) and depression that begins after the baby is born (called postpartum depression).
Baby blues is a term used to describe mild mood changes and feelings of worry, unhappiness, and exhaustion that many women sometimes experience in the first 1 or 2 weeks after having a baby which is normal.
If mood changes and feelings of anxiety or unhappiness are severe, or if they last longer than 2 weeks, a woman may have postpartum depression. Women with postpartum depression generally will not feel better unless they receive treatment.
Further information on the signs and symptoms of baby blues, PPD and PD can be found on the websites of U.S. National Institute of Mental HealthExternal link and nonprofit American academic medical center Mayo ClinicExternal link.
Undetected and untreated
While suffering from depression, Quantius started doing research on screening, treatment and support of mental health conditions during major life transitions for women. She had extensive experience in the field of computational biology, drug discovery and treatment optimisation.

“It was only after conducting an informal online survey through social media channels that I became fully aware of how neglected and underserved this issue is,” she says.
Women from all over the world reached out to Quantius through her survey with their stories of undetected and untreated perinatal depression. She learned that undetected perinatal depression could lead to long-term consequences, such as suicide and even infanticide. She also noticed a huge lack of access to screening in low and middle-income countries, such as her native India. There 22% of women are estimated to suffer from perinatal mood disorders, but there is no dedicated maternal mental health regulations available.
But even higher-income countries like Switzerland struggle to screen for the condition in a timely manner; when Quantius moved to the Alpine nation, she realised that the screening was no better than in the US – in fact, Switzerland ranks far behind other Western countries when it comes to routine screening and timely treatment of the condition.
Andrea Borzatta, president of the advocacy group Postpartale Depression Schweiz (Postpartum Depression Switzerland)External link, believes that the problem lies in a shortage of professionals and lack of expertise. She says the issue is especially acute in French and German-speaking regions, where there are only a few specialised professionals and hardly any communication in the field – something her organisation is working on remedying.
“The online training we organised for professionals in Switzerland demonstrates that many healthcare professionals don’t know how to discuss PDD with the person affected. They are worried about aggravating the depressive symptoms of the patients or scaring them.”
Some professionals also downplay the depressive state of new mothers, says Borzatta. All new parents are affected to a greater or lesser extent by many symptoms of physical exhaustion. The distinction between so-called “baby blues”, a normal emotional state, and the serious condition of PPD is unclear for many professionals, adds the Swiss psychotherapist Claudine Haus.
Anke Berger, a lecturer at the Bern University of Applied sciences focusing on research of perinatal mental disorders in Switzerland, points out that the prevalence of postpartum depression– currently about 13,000 women per year – would probably be significantly higher if those untreated and undetected were included.
“The topic of perinatal depression is still not addressed consistently and with sufficient time in all prenatal classes in the country. Besides, after childbirth, consistent and repeated screenings of all mothers and fathers for postpartum mental illnesses are absent,” says Borzatta.
Bridging the gap
So how can women identify what they are experiencing and seek help if needed? Currently, there are numerous self-tests online to determine whether women have perinatal depression symptoms. But these quizzes are no substitutes for a formal diagnosis which has to be made by licensed mental health professionals or doctors.
The Edinburgh Postnatal Depression Scale (EPDS) is a set of 10 screening questions that can indicate whether a parent has symptoms that are common in women with depression and anxiety during pregnancy and in the year following the birth of a child.
EPDS is not a diagnostic tool – rather it is a screening tool that aims to identify women who may benefit from follow-up care, such as mental health assessment, which may lead to a diagnosis based on accepted diagnostic criteria.
Advantages: EPDS is very user-friendly and takes only about 5 min to complete. And it has been translated into many languages.
Disadvantages: The questionnaire may be used incorrectly, e.g. too early (indicating baby blues but not yet depression) or confused with a fixed diagnosis.
Another possible disadvantage is that EPDS focuses too much on the classic symptoms of depression. However, there are other mental disorders such as obsessive-compulsive disorder, anxiety disorder, attachment disorder, Post-traumatic stress disorder that occur postpartum but couldn’t be well assessed with EPDS.
Swiss association Postpartale Depression Schweiz offers EPDS online self-test in 17 languagesExternal link.
Other self-test tools for perinatal depression: Postpartum Depression Screening Scale (PDSS), Patient Health Questionnaire (PHQ-9), Beck Depression Inventory-II (BDI-II), Depressions-Angst-Stress-Skala für die Peripartalzeit (DASS-P), Mental Health Inventory (MHI).
Source: Andrea Borzatta, Postpartale Depression Schweiz
Many women with PPD are also reluctant to receive face-to-face counseling. They suffer in silence because they are ashamed of their feelings and don’t want to be seen as ungrateful for the care of their doctors and midwives, says Borzatta.
For that reason, Quantius wants to find another way to screen for perinatal depression that involves a “more holistic and evidence based perinatal care”, as she puts it.
This drive led her to quit her job as director of computational biology in the pharmaceutical industry and join the Federal Institute of Technology in Zurich (ETHZ) as a senior scientist to develop a digital diagnostic tool called “Haplomind”. It uses data analytics, digital phenotyping and machine learning to identify and help treat women experiencing depression and anxiety anytime from pregnancy to the end of the first year after the birth of a child.
Haplomind can be used by pregnant or postpartum women together with their gynecologists, obstetricians and midwives. It aims to empower women to create their own digital evidence base for further treatment, on their own terms. Women can record how they feel during pregnancy and the postpartum period, and how they feel after taking medication or after therapy.
Quantius hopes that the data gathered from the app can help the healthcare system improve personalised screening and create an evidence base for individual treatment. By interpreting the self-reported data from mothers, professionals are trained to diagnose the level of perinatal depression, and which treatment – self-directed, peer-supported, medical or alternative treatments – would most likely be used.
More
Treating mental illness in pregnancy ‘still a grey area’
Confidentiality of personal health data
Many app users, especially users of health-related apps, are concerned about data privacy and how the information they share will be used. If women are not comfortable discussing PPD with medical professionals can they really be expected to share their experiences with technology platforms that have a reputation for harvesting user data? Quantius stressed the importance of privacy and security of users’ personal health data when they use Haplomind and other digital health apps.
“Women can only overcome the stigma around depressive disorders and discuss mental health issues with professionals if we create an easily accessible, secure and trusted space,” she says.
Haplomind is cooperating with Ernst HafenExternal link, co-founder of MIDATAExternal link, a citizen-owned data trustee model. This model ensures that users are the only persons who can grant third parties (e.g. medical research projects) access to their datasets. Currently, Haplomind is testing the feasibility of the app prototype in a pilot study with the Indian National Institute of Mental Health & Neurosciences (NIMHANS) in Bengaluru, India, supported by a grant from ETH for Development.
Quantius is also planning to test the feasibility of this app in collaboration with the University Hospital Zurich in Switzerland and is working with researchers in Canada and New Zealand to introduce the digital solution there. Her ultimate goal is to help new mothers and pregnant women get screened on time and find reliable resources for those feeling through depressed or anxious during or after pregnancy and also create an ‘perinatal specific evidence base’ that empowers women to take care of themselves and also helps the healthcare professionals to personalise treatment options specific to the individual.
“PPD shouldn’t be a stigma that prevents women from seeking timely help, or the reflection of what kind of mother you are. Testing and treating PPD should be as common as routine physical examinations during pregnancy and post-partum,” says Quantius.

In compliance with the JTI standards
More: SWI swissinfo.ch certified by the Journalism Trust Initiative



You can find an overview of ongoing debates with our journalists here . Please join us!
If you want to start a conversation about a topic raised in this article or want to report factual errors, email us at english@swissinfo.ch.