Vaccines – a triumph of hope over delivery

For the past 50 years, the search for a vaccine has been the holy grail of malaria research.
Several studies have convinced scientists that a vaccine is feasible, yet they are still far away from a final product.
The problem is the ingenuity of the malaria parasite. It may only be single-celled but during the course of its lifetime and particularly while it is in the human body, it changes its forms, its hiding places and even its surface structure.
Vaccines work by stimulating the immune system to produce antibodies to an apparent threat. When the real thing comes along, the immune system responds much more quickly and takes out the invader before it causes serious damage.
Ideally a malaria vaccine would prime the immune system to destroy all parasites, whether free swimming in the blood, in the liver or even in red blood cells.
Researchers are now beginning to accept that they may have to lower their sights, but they remain optimistic thanks to some intriguing observations.
Proof of principle
It has been known for 30 years that if you take a mosquito infected with sporozoites and expose it to radiation, you weaken the parasites inside the mosquito, removing their ability to replicate.
When the mosquito bites you, these irradiated parasites travel to your liver where they simply generate a response from your immune system. If a mosquito with a healthy malaria parasite bites you, the body will spend several months killing off the invader.
Unfortunately, the technique is highly impractical outside research laboratories as it can take a thousand bites from irradiated mosquitoes to induce immunity.
“It’s an important proof of principle and that’s why we still work on vaccine development,” explains Marcel Tanner, director of the Swiss Tropical Institute.
Another factor that inspires hope is that people living in endemic areas acquire partial immunity with age following continuous exposure to infected mosquito bites.
“We should be able to do through a vaccine what the human body learns through long-term exposure,” says Tanner.
Finally, immunoglobin purified from the blood of individuals who are life-long residents of endemic regions has been used to successfully treat severe malaria infections in young children.
These antibodies prevent the parasite from invading new red blood cells and significantly increase their clearance by the spleen.
Immune response
Some scientists are experimenting with a vaccine, which attacks the parasite when it is breeding in the liver and before it invades red blood cells.
Lausanne-based start-up, Dictagene, has adopted this approach. The company has observed a protein or antigen on the surface of the malaria parasite, which protects mice and monkeys against the disease.
It has therefore created a synthetic protein fragment, which mirrors the action of this substance in the body in triggering an immune response.
Meanwhile, other researchers are looking at a vaccine that makes it difficult for the parasite to multiply in red blood cells. This would not stop infection but would limit the severity of the disease and help prevent deaths.
A different tack is a vaccine, which doesn’t prevent you from getting sick, but stops the parasite from developing in the mosquito.
The idea is that when the female mosquito takes a meal of infected blood, she also ingests antibodies, which protect her from becoming infected. As a result, she is no longer able to spread malaria.
Yet another initiative is seeking ways to prevent the parasite from travelling from the gut of the mosquito to the saliva, where it can infect man.
Cocktail
A vaccine aimed at one stage of the parasite’s life cycle will not necessarily stop the other stages.
A sporozoite vaccine might protect against the infectious form injected into a person by a mosquito, but if a single sporozoite was to escape the body’s immune defences, it could still lead to full blown disease.
Experts believe that the ideal product will be a cocktail of vaccines aimed at different stages of the parasite’s life cycle and perhaps also at two or more species.
Most vaccine efforts are directed towards falciparum malaria because of its severity but four different species of parasite cause human malaria.
Perhaps a short-term vaccine for travellers to prevent infection will differ from a vaccine aimed at populations in endemic areas, designed to reduce the severity of the attack.
Field trials
The Swiss Tropical Institute has been involved in two important malaria vaccine trial programmes in endemic regions in the last six years.
The institute collaborated on the Tanzanian trial of the SPf66 candidate vaccine whose results proved disappointing but which offered valuable experience.
They also collaborated in trials with a cocktail vaccine of three antigens in Papua New Guinea, which had a significant effect against parasite densities – the best so far in the field.
Whether a vaccine will finally be available – let alone produced on a large scale and distributed to poorer countries – remains, however, an open-ended question.
“I think we’ll get a malaria vaccine,” says Robert Ridley of the World Health Organization’s tropical disease research programme. “I don’t know when that will be.
“Estimates vary from ten years if you are optimistic, to 30 years if you are less optimistic, to never if you are really pessimistic. All of those options are probably equally valid scenarios.”
swissinfo, Vincent Landon
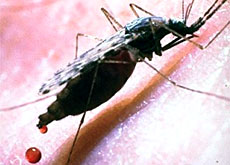
Malaria is transmitted through the bite of a female anopheles mosquito.
Microscopic parasites enter the victim’s liver and reproduce over seven to ten days.
The parasites break out from the liver and invade red blood cells where they multiply.
Every 48-72 hours the red blood cells rupture, freeing the parasites to attack again.
A female anopheles feeds on the patient.
The parasite takes at least eight days to develop in the mosquito.
The mosquito bites another human, injecting infected saliva.

In compliance with the JTI standards
More: SWI swissinfo.ch certified by the Journalism Trust Initiative










You can find an overview of ongoing debates with our journalists here . Please join us!
If you want to start a conversation about a topic raised in this article or want to report factual errors, email us at english@swissinfo.ch.