
Fight over rights to Covid-19 drugs puts Switzerland in a tough spot

Switzerland is caught between established practice and global solidarity when it comes to paying for and rewarding medical innovation.
The Alpine country’s economy and its self-professed identity as an innovation powerhouse rely heavily on the rights and rewards attached to patents. It has the most European patent applications per capita and performs well in rankings of patent quality, a large portion of which are in the biomedical field.
This is why recent calls by global health advocates and some governments to loosen patent protections during the Covid-19 crisis to make drugs and vaccines widely available have caused some unease in Switzerland. As more countries back a more flexible patent regime for Covid-19, Switzerland is finding itself pitted between industry on the one hand and global solidarity on the other.
At the World Health Assembly in Geneva a couple of weeks ago, the Swiss government supported a resolution that called for the “voluntary pooling and licensing of patents to fight Covid-19”. But other calls to override or eliminate patents completely through compulsory licensing, open licensing or a so-called “People’s VaccineExternal link” have not been as welcome.
“Switzerland takes intellectual property rights very seriously and will not undermine the regime so easily,” Gaétan de Rassenfosse, a professor of Innovation and intellectual property policy at the Federal Institute of Technology in Lausanne (EPFL), told swissinfo.ch.
While the global debate is centred on the current crisis, breaking entrenched views and laws on patent protection could open the door to debate about patents in other areas such as cancer and rare diseases where prices have become prohibitive for some public health systems.
Familiar territory
Many in public health circles look to what happened when HIV drugs came on the market a couple decades ago as a precedent. Market exclusivity kept prices so high that less affluent countries, which had the greatest need for the drugs, were effectively shut out.
In 2001, Basel-based Roche dropped the price of its HIV drug Nelfinavir by 40% after the Brazilian government threatened to use compulsory licensing, a clause in intellectual property lawExternal link that allows countries under certain conditions to grant licenses to public health agencies or generic manufacturers without the consent of the patentholder.
Covid-19 is bringing the issue back to the forefront with added urgency as billions in taxpayer money, including from Switzerland, is funneled into vaccine research and clinical trials. This has created a nationalistic domino effect as a growing number of countries stake claims on R&D efforts.
Paris-based pharma company Sanofi found itself backtracking under pressure from France after its CEO said the US government had the right to the largest pre-order of an eventual Covid-19 vaccine “because it’s invested in taking the risk”.
More
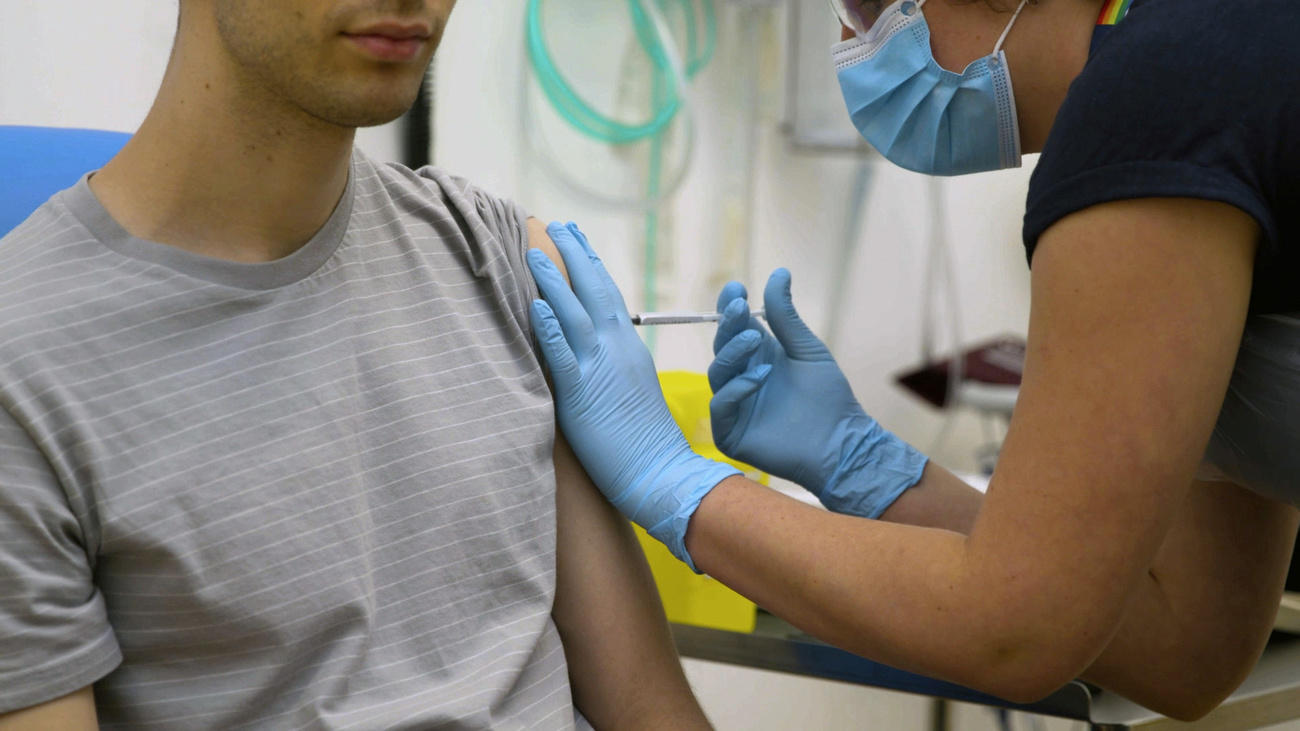
Government earmarks CHF300 million to secure Covid-19 vaccine
Questions have been raised in Switzerland about whether it will have first dibs on any diagnostics, treatments or vaccines discovered or produced on Swiss territory by the likes of Roche or Lonza. The government announced last week it is negotiating with manufacturers, setting aside CHF300 million to secure access to a vaccine for the population.
Holding the cards
While governments jockey to secure special access to any promising solutions, most big pharma giants working on Covid-19 products are trying, at least publicly, to stay out of the crosshairs by talking up the industry’s “unprecedented collaborationExternal link” and the need for solidarity.
“I sense a real responsibility among industry leaders,” said Thomas Cueni, who heads the Geneva-based International Federation of Pharmaceutical Manufacturers and Associations (IFPMA). “We don’t want to run lotteries on who gets our medicines and our vaccines.”
Cueni said that the leaders of Switzerland’s pharmaceutical companies were aware that demand for new treatments and vaccines could outstrip supply, but they would strenuously fight the loosening of their patent protections.
Instead, companies were exploring bilateral voluntary licensing and existing mechanisms such as the Medicines Patent PoolExternal link that focus on access for poorer countries, as part of the “arsenal of options to make any Covid-19 products accessible,” Cueni said.
Pharma giants also hope to ward off questions about patents by boosting supply. A Roche spokesperson told swissinfo.ch that it is ramping up production of the arthritis drug Actemra, which is currently in clinical trials against Covid-19, and aims to more than double production of its new coronavirus antibody test to more than 100 million tests a month by the end of the year.
Still, the company admits that demand for tests “will exceed supply for the foreseeable future” and encourages countries to prioritise distribution for those who show clear symptoms.
Bargaining chip
Patrick Durisch from Swiss NGO Public Eye argues that relying on voluntary acts by industry could hamstring the global response to the pandemic. “It is in the public and global interest to have as many producers as possible and make Covid-19 solutions available where they are needed,” he said.
“Companies are trying to show goodwill with drug donations and sharing their libraries of molecules, but they don’t want to give up control of manufacturing and patents.”
Public Eye is one of more than 70 organisations and individuals calling on governments, including Switzerland’s, to support the pooling of rightsExternal link and open licensing for all technologies necessary for the prevention, detection and treatment of Covid-19.
These include not just the recipes for drugs but also “trade secrets” including technology and manufacturing processes, Durisch said.
Innovation expert de Rassenfosse argues that companies are unlikely to give up control. “It is most likely that [companies] will use patents as a bargaining chip with individual governments or to receive some compensation. If they don’t patent, they will be left with nothing to exchange,” he said.
Some companies have already signed dealsExternal link with manufacturers in Asia for patented drugs in effect side-stepping open licensing.
The Swiss Federal Institute of Intellectual Property (IPI) has already received more than a dozen patents applications related to Covid-19 since the crisis began, a spokesperson told swissinfo.ch. It is unclear how many of these came from the biomedical sector.
The European Patent Office declined to share patent application findings related to this coronavirus outbreak, arguing that it was too early to release such information and noting that patent applications remained confidential for 18 months.
Weighing the risks
In some other countries, companies may have no choice but to share their findings. Germany and Canada amended laws to facilitate compulsory licensing during the coronavirus crisis. Israel also issued a permitExternal link allowing it to import a generic version of AbbVie’s Kaletra from India for coronavirus patients.
De Rassenfosse says while legal, the proposition carries risk for Switzerland. “Any country that aggressively forces companies to give up patent rights should expect a change in the enthusiasm of companies for that market,” he said.
Cueni told swissinfo.ch that compulsory licensing is an “extraordinary measure” and should not be used as a threat or routine policy tool, as it has a “chilling effect on innovation”. A spokesperson for the Swiss federal public health office also told swissinfo.ch that the office considered it as a “means of last resort.”
Prior to the pandemic, many companies were shunning R&D in vaccines and antibiotics because they offered little prospect for profits.
More
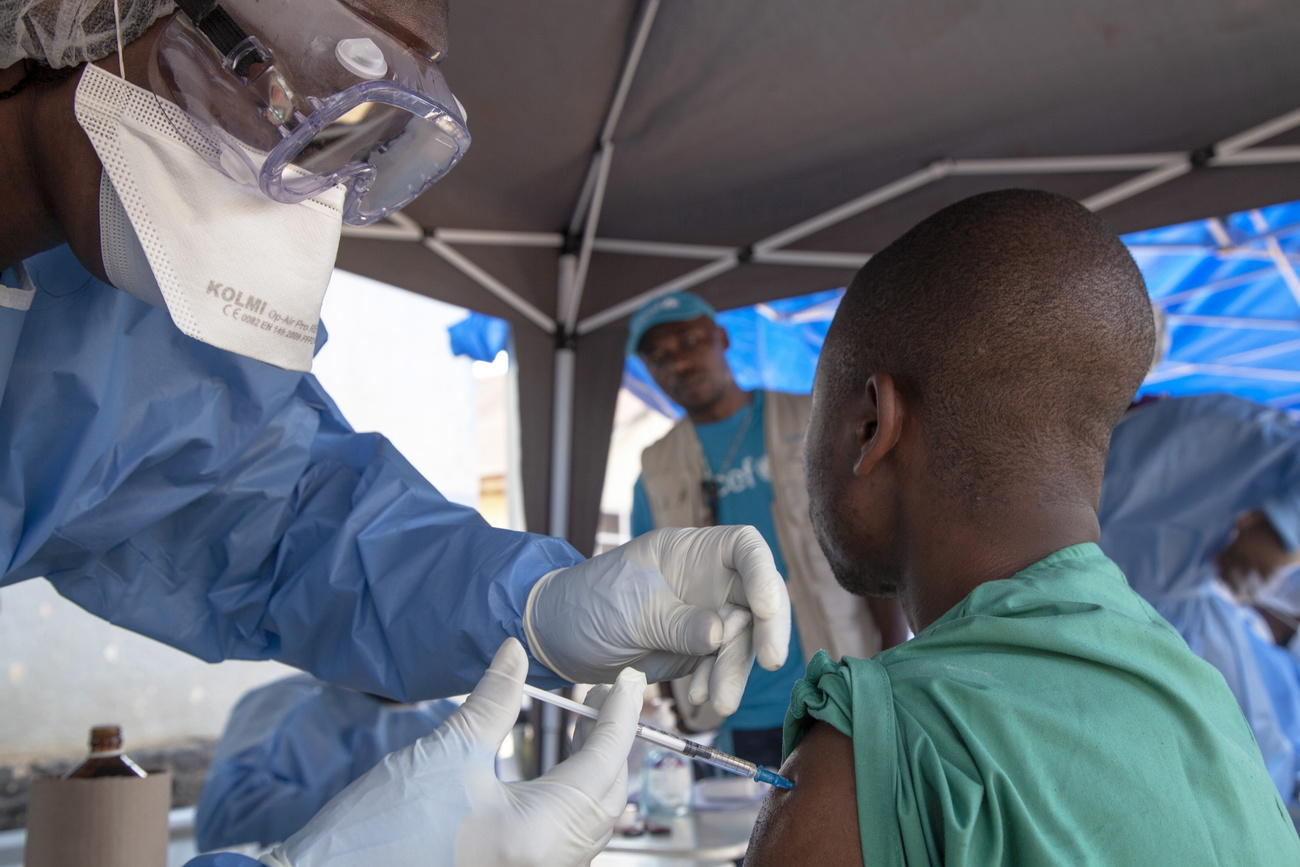
With no prospects for profits, big pharma neglects new infectious diseases
Felix Addor, the General Counsel at IPI told swissinfo.ch that “private companies could withdraw from or trim their R&D activities for vaccines or treatments against Covid-19 if countries issue or even threaten compulsory licenses. This is definitely not what Switzerland is aiming for.”
Cooperation with patent holders, adds Addor, is a more promising and efficient way to find effective medicine. By granting licenses for others to manufacture, it can bring down the price without reducing the patent law.
Innovation conundrum
The debate is raising a more fundamental question: Are patents good or bad for innovation?
Roche didn’t say if it was willing to participate in a global technology pool, but a spokesperson told swissinfo.ch that “intellectual property protection is essential for medical innovation and is needed to address the healthcare challenges we face today.”
Companies pour billions into research, sometimes over decades with – in some cases – a 1% chance of being successful, according to their own estimates. “The whole system is built on the basis that innovation is rewarded by a limited exclusive right to the market,” said Christian Moser, a patent expert at IPI. “That inventors should be able to exploit innovation and to prevent others that are not innovative, but are simple copycats.”
He acknowledges that the relationship between patents and innovation is not black and white. For public health advocates like Katy Athersuch, a policy advisor with Médecins sans Frontières in Geneva, patents are part of a proprietary approach when what we need right now is global solidarity.
“We need complete sharing of everything that could help scale up manufacturing and enhance R&D so that we aren’t holding back any information that is helpful to our global response to Covid-19”.
At this point, given the range of research activities under way on patented and off-patent drugs as well as new and old drugs, Esteban Burrone from Medicines Patent Pool, says it makes sense to keep the options open.
“We are all trying to understand how to make therapies available rapidly to as many people as possible whenever there is proven efficacy,” said Burrone.

In compliance with the JTI standards
More: SWI swissinfo.ch certified by the Journalism Trust Initiative































You can find an overview of ongoing debates with our journalists here . Please join us!
If you want to start a conversation about a topic raised in this article or want to report factual errors, email us at english@swissinfo.ch.