
Overwhelming, lonely and stressful – life in the Covid-19 unit in Geneva
As her time working in Geneva University Hospital (HUG)’s Covid-19 intensive care ward comes to an end, Médecins Sans Frontières’ (MSF) nurse Kathrine Zimmerman, who was seconded to the hospital, reflects on her daily life at the height of the pandemic.
When I arrive for my shift in the evening, I discover the unit to which I will be assigned for the next 12 hours. At first, the crossover between those starting and ending their shift is impressive as there are so many of us. At the entrance of the changing rooms, it’s time to choose and put on my uniform for the night.

The size can vary but not the colours: blue and white. As soon as we enter the areas where patients are intubated, we put on FFP2 masks or “duck bill” masks. In the corridors, as a precaution, we still wear conventional masks to protect each other. After two-and-a-half weeks on duty in the Covid-19 unit, I spent one night in an intensive care unit for non-COVID patients, dressed normally with a normal surgical mask. It was very strange to be without all that clothing, I felt almost naked.
My small contribution
When the pandemic was declared and cases were admitted to hospitals in Switzerland, I could hardly see myself working from home, especially when I had the opportunity to help reinforce the hospital teams. Although I did not necessarily imagine I would ever be responding to an epidemic of such magnitude in Europe, I am happy to be able to contribute, at my level, to this incredible mobilisation. At the HUG, intensive care has been extended over several buildings. Operating rooms, recovery rooms, intermediate care rooms and other services have been reassigned to receive patients with Covid-19.
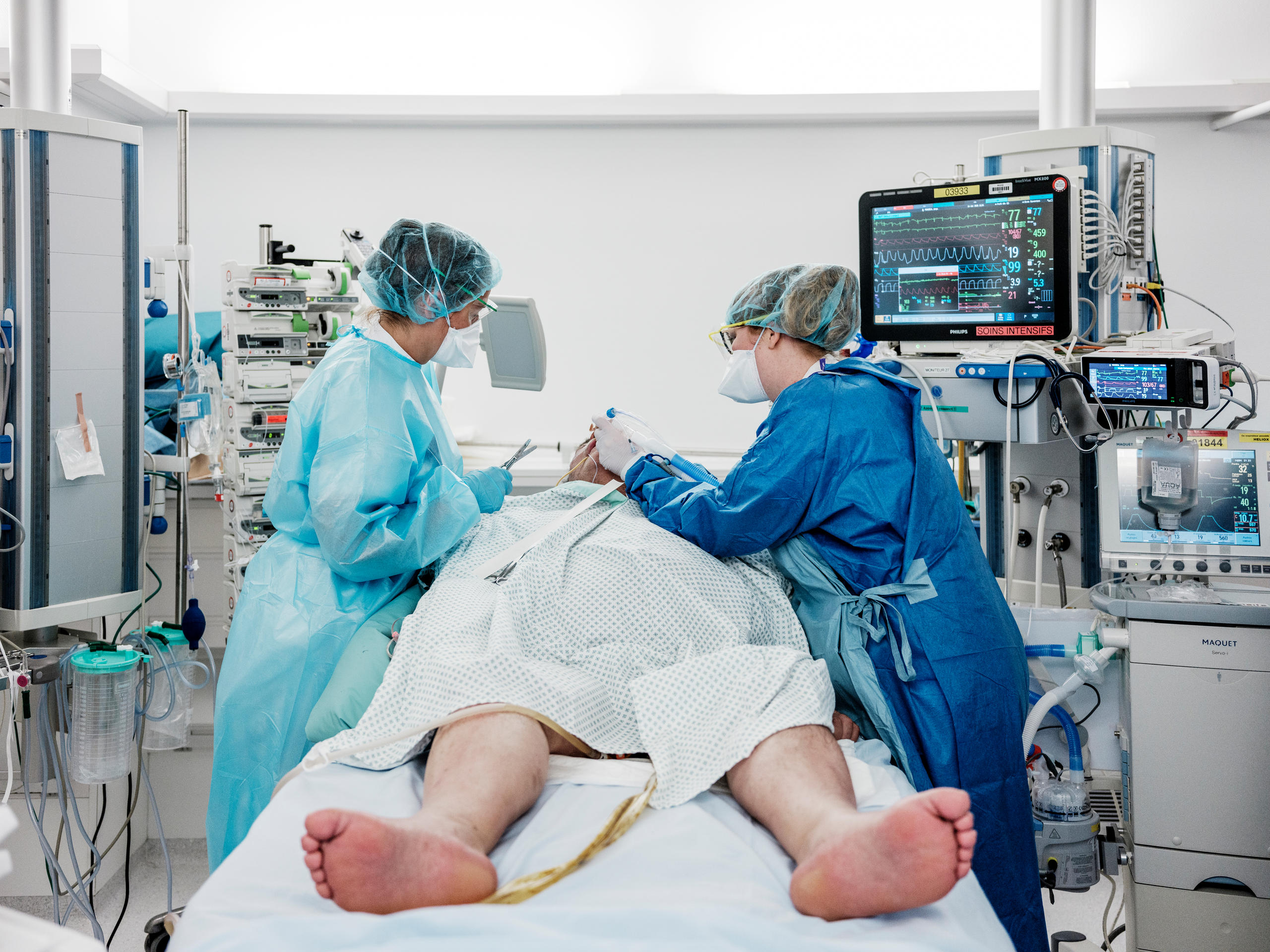
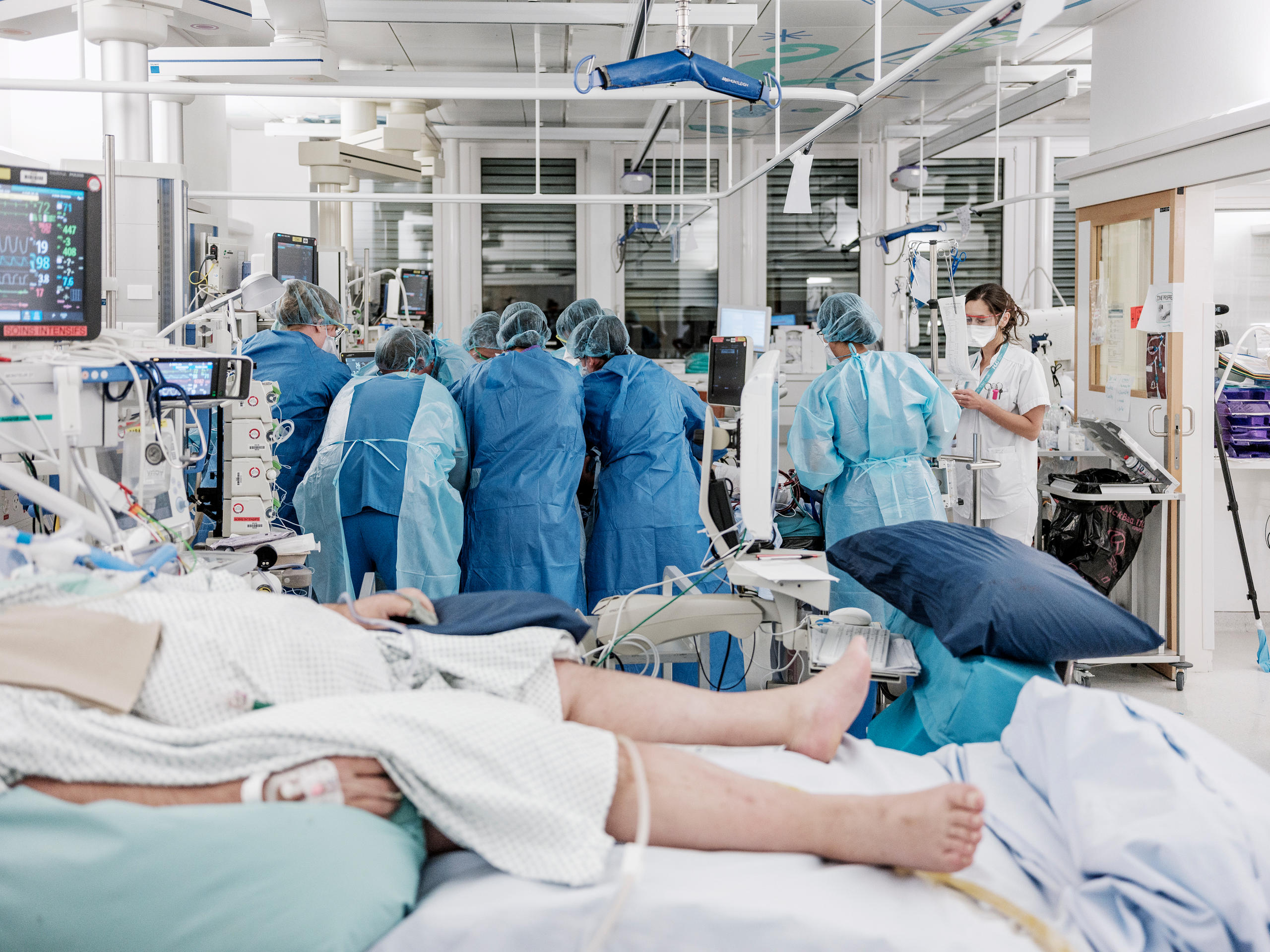
For the first two weeks, I cared for several “young” patients under the age of 55, many of whom were able to be extubated and moved up to the continuing care floor. Some were discharged a few days later. This positive news is what keeps us going. All the same, seeing so many people intubated, often lying on their stomachs to improve their breathing, is overwhelming. You don’t usually see that many intubated patients in the ICU. They are all here, and when I arrived, we were told that depending on the evolution of the crisis, we could potentially have five intubated patients per nurse. I ended up with three of them on my first day and I must say it was very stressful to find myself in an unknown ward after several years outside of intensive care. Luckily, it didn’t come to that point and the situation is actually improving.
One thing that particularly strikes me about this extraordinary experience is the loneliness of the patients. The healthcare staff, nurses and doctors are the only link between patients and their families. A few days ago, one of the patients I was caring for was also celebrating his birthday (we share the same birthday). I was able to celebrate with my family, even if it was via Skype. He spent his 80th birthday alone. And his family too. That’s tough. I’ve since learned that he was extubated. I hope he’ll be reunited with his family soon.
Similarities with my humanitarian experiences
I see parallels with my years of experience in the field with how worried people become with the disease: panic, stress, struggling with this epidemic environment, and the concerns of my colleagues and myself.
I am following the situation from a distance, but I know that my MSF colleagues are preparing themselves in the field and helping to implement preventive measures so that the disease does not spread and overwhelm health systems that are less well equipped than the ones in Europe. However, there will be a lack of human resources for patient treatment, not to mention the need for staff specialised in resuscitation. It will not be possible to provide the same level of care as here. Restrictions on the movement of people and goods will complicate the implementation of the response.
We already feel somewhat helpless and limited in what we will be able to provide, even if we do what we can to apply the best possible care protocols.
The field? I’m a little bit there right now.
These days I live in a bubble and my main concern is to look after the patients I am responsible for. Nonetheless, when I think of my humanitarian colleagues working in the field, I know it’s going to be difficult. I’m not sure I would easily go help with a Covid-19 response in another country. What is certain is that I would take the time to consider it seriously.
In Switzerland, I feel like I’m a little bit in the field given the reaction of my friends and family who tell me: “Now that you are no longer in a dangerous country, you just had to get into Covid!”. Fortunately they trust me.
This blog was originally published on MSF’s Voices from the field blogExternal link.
When the virus started spreading in Switzerland, at the end of March MSF deployed 12 specialists in Geneva helping the main hospital as well as the homeless and other vulnerable residents.
In Geneva, an MSF mobile clinic continues regular visits to the Vernets military barracks where vulnerable residents are living to carry out contact tracing activities. Otherwise demand for MSF activities has reduced as the spread of the virus has reduced.
Infection prevention control support is also being provided to different local associations upon request. On May 2, 25 MSF volunteers conducted a survey of around 2,500 vulnerable people attending a food distribution in Geneva. A medical booth handled by MSF & HUG medical staff offered free Covid-19 tests. In the Haute-Savoie region in neighbouring France, a small MSF team has provided medical support to structures and associations in Annecy and Annemasse.

More
MSF deploys Covid-19 teams in Geneva to help most vulnerable

In compliance with the JTI standards
More: SWI swissinfo.ch certified by the Journalism Trust Initiative































You can find an overview of ongoing debates with our journalists here . Please join us!
If you want to start a conversation about a topic raised in this article or want to report factual errors, email us at english@swissinfo.ch.