
Solving the ventilator shortage
ETH Zurich researcher Torbjørn Netland advocates a global approach to the production of ventilators and defines six areas of activity.
An epidemic is an emotional issue. With the lives of our friends and loved ones on the line, our reaction tends to be: Close the borders! Ground the planes! Such responses are natural and perfectly understandable.
The virus doesn’t worry about boundaries – and nor should we
Although isolation has become a necessity on a personal level, using the same strategy in other contexts can quickly become counterproductive – for example, when it comes to ventilators.
Health ministries all over the world face the same dreadful dilemma. Last year, 77,000 new ventilators were enough to meet the market demand of the entire planet. In April, New York City alone forecasts a need for 30,000 additional machines – and no one has a real idea of what the total demand in the corona crisis will be.
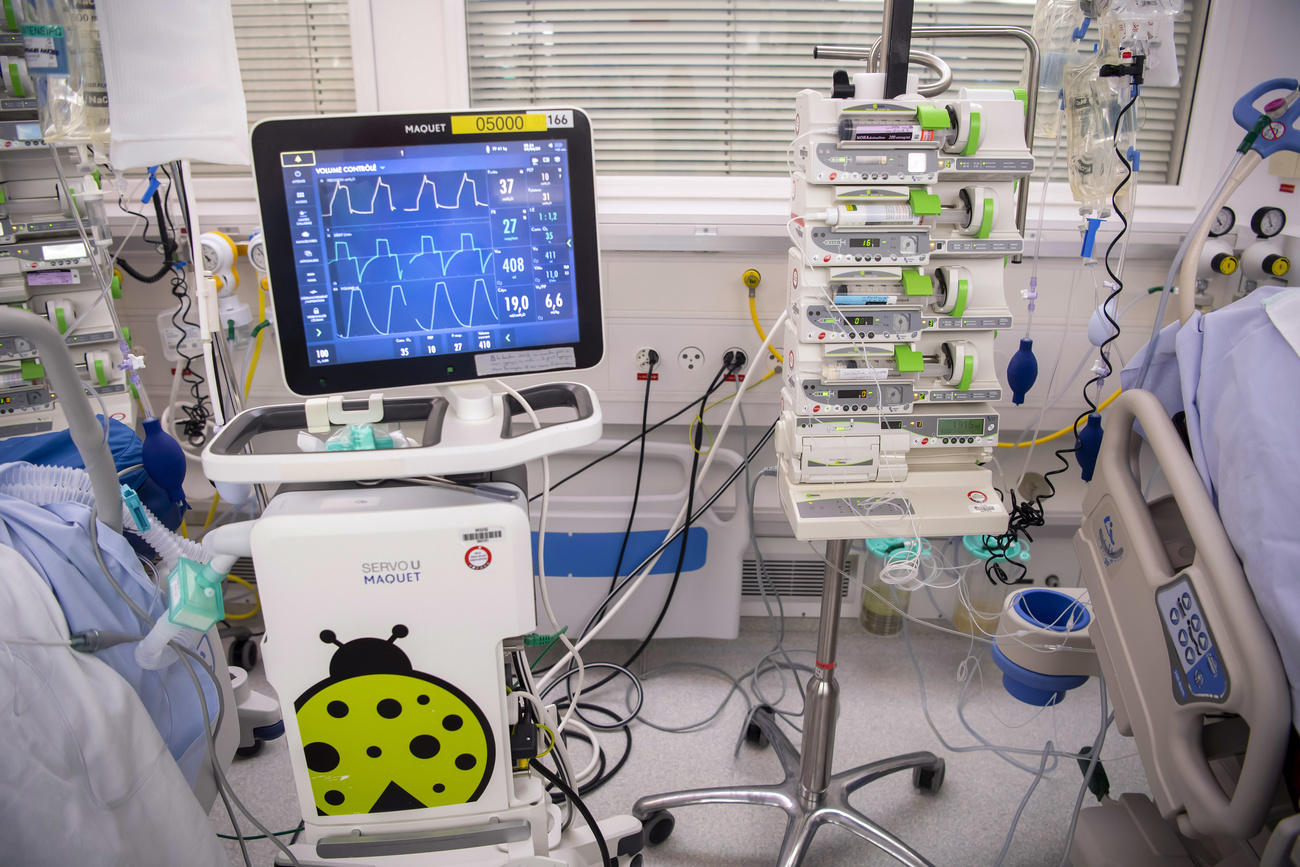
Where will we get all these machines?
Short-sighted politicians everywhere see increased domestic production as the solution to the ventilator shortage, and for some products and some countries that may well be part of the solution.
But when you look at where the ventilator companies are located and where they source the 700+ parts that go into them, it’s easy to see that a better solution is not hoarding machines, 3D printing, or cobbling together makeshift contraptions. In the short run, the only way to succeed is by getting the world’s most established ventilator manufacturers to mass-produce many more units. Fast.
Unfortunately, the global supply chains – which we could use most now – are being dismantled. Such systems are now even discredited as one of the factors triggering the pandemic. Do we want to save the lives of as many coronavirus victims as possible? Then we should increase the worldwide production capacity of ventilator manufacturers, not hinder it.
All pulling together
The leading manufacturers of ventilators have the advantage of not having to convert their entire production lines. They can also produce more cost-efficiently.
But there is a catch: although some of these manufacturers have already increased their production by 30-50%, they cannot achieve a growth rate of 500 or 1,000% alone, which may be the level required.
They need support with their supply chains. I am not suggesting that the WHO should coordinate the entire production capacity and transport of ventilators.
But the producers and the supply chains of ventilators, large logistics companies, the national postal services and even the national military procurement agencies should work together.
Six areas of activity
First, let’s map the supply chain for ventilators. In normal times it is enough to partner with reliable subcontractors, but in a crisis, manufacturers need to know what parts are needed and where they can be procured. Which components are the most scarce? Is the component necessary, or can a more readily available alternative be used instead?
Second, let’s streamline the pathways. Consider the best ways to get those parts to the manufacturer, and what it would take to expand capacity. Is there any overlap in supply chains between industries, for example, that could facilitate easier shipments? Could we establish global, rapid-response logistic networks through air traffic hubs?
Third, let’s forecast demand. Plot where demand is growing, and where the next coronavirus epicentres are likely to be. Leading research centres such as Imperial College London are already contributing daily updates, and their analytics could be used to manage orders fairly and efficiently.
Fourth, let’s recruit more help. Next, think about which companies, at each level of this supply chain, are best positioned to step up their capacity. In the United Kingdom a vacuum cleaner producer is ramping up production of a new device designed in house. Who else might have useful expertise?
Fifth, let’s train the operators. One manufacturer said recently in Der Spiegel that the biggest challenge is to find enough trained people to operate the ventilators. Can the machine be simplified and made more user-friendly?
Does the documentation need to be improved or training simplified or digitalized? Could we start training health care workers now to run the ventilators that will arrive in the next few months?
Sixth, let’s look for alternatives. The above tasks should take priority, but during this global crisis, we must also look for substitute products. Many ambulances have respirators as part of their standard equipment. For the duration of the emergency, reserve mobile respirators could be re-purposed.
Could lower-tech solutions, such as hand pumps, which saved lives in Copenhagen during a 1952 polio epidemic, play a role in some countries?
Finally, we must not lose sight of this global, strategic view throughout the entire duration of the emergency. If we want to solve the health problems caused by the Covid-19 pandemic effectively and efficiently, we must adopt a broad, systemic perspective. The virus doesn’t worry about boundaries – and nor should we.
This blog was originally published on the ETH Zurich’s ZukunftsblogExternal link, as well as on the World Economic Forum’s AgendaExternal link.
The views expressed in this article are solely those of the author, and do not necessarily reflect the views of swissinfo.ch.
Opinion series
swissinfo.ch publishes op-ed articles by contributors writing on a wide range of topics – Swiss issues or those that impact Switzerland. The selection of articles presents a diversity of opinions designed to enrich the debate on the issues discussed.

In compliance with the JTI standards
More: SWI swissinfo.ch certified by the Journalism Trust Initiative































You can find an overview of ongoing debates with our journalists here . Please join us!
If you want to start a conversation about a topic raised in this article or want to report factual errors, email us at english@swissinfo.ch.