
From Covid to Hormuz, what has Switzerland learned about drug shortages?

The conflict in the Middle East has wreaked havoc on global supply chains, including those of the pharmaceutical industry. Is Switzerland applying lessons from similar challenges experienced during the Covid-19 pandemic?
The blockade of the Strait of Hormuz over the past month has disrupted supply chains and affected the transport of a quarter of the world’s gas, leading to a sharp rise in fuel prices. The International Energy Agency said the world is enteringExternal link “the greatest global energy security threat in history”, while the World Health Organisation warned of knock-on effects across sectors, including essential medicines and supplies.
In Switzerland, the latest report by the Federal Office for National Economic Supply (FONES), which monitors shortages in essential goods such as energy and food, said none were at risk of shortages – except therapeutic goods, defined as essential pharmaceuticals, medical devices and hygiene products. These were marked in the April 15 FONES report by a yellow box, meaning the availability of some essential pharmaceutical ingredients was “limited”.
+ Switzerland is known for its pharmaceutical industry. So how come medicine is unavailable?
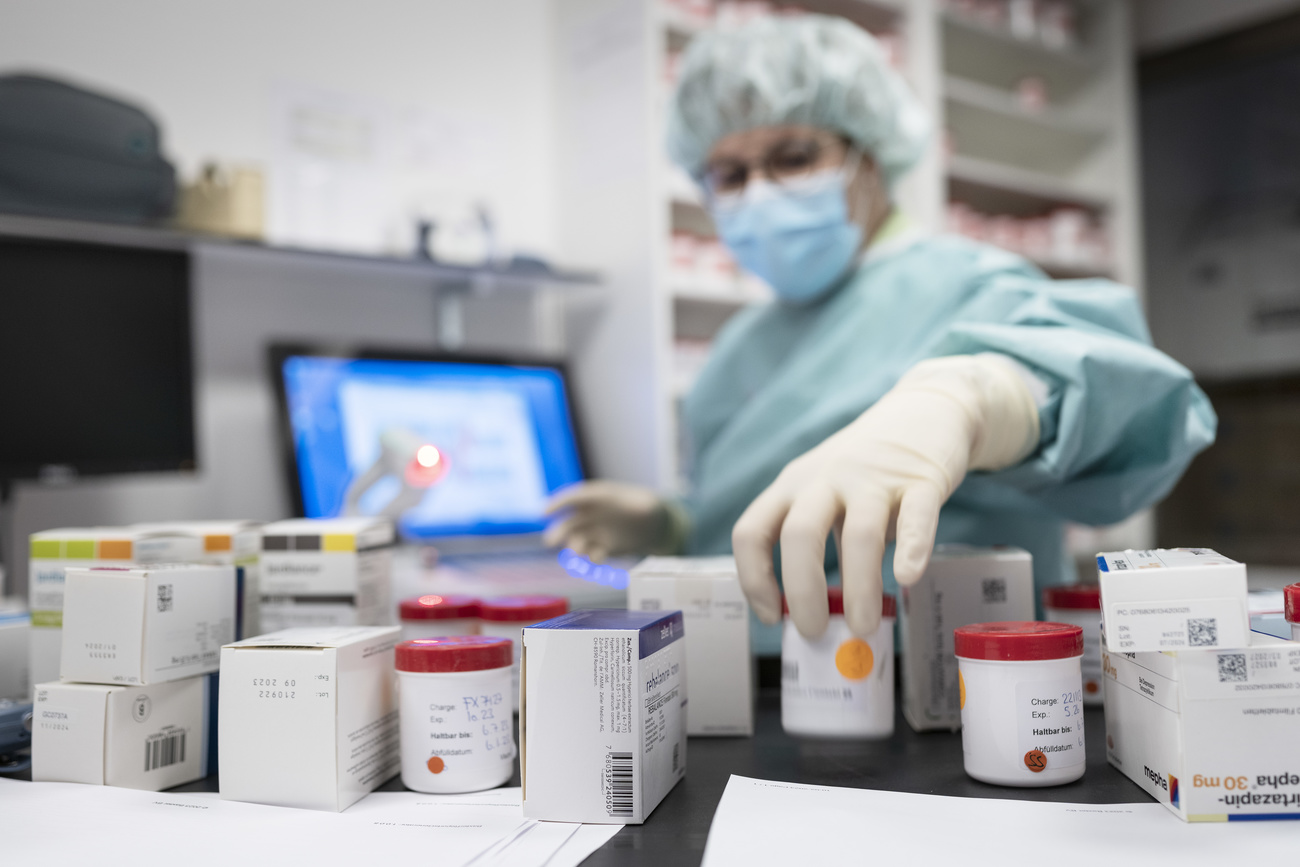
More
Why Switzerland is running out of pharmaceuticals
This category of goods has been marked yellow since FONES began colour-coding shortages in May 2025 – about 140 essential pharmaceuticals are currently unavailable in Switzerland. They are part of a broader group of over 500 prescription drugs unavailable due to the pharma industry’s dependance on just a few markets for goods. Production lines have been further weakened by the conflict in the Middle East: it has delayed delivery of chemicals central to drug and medical equipment manufacturers in China, slowed production in India, and led to higher global shipping costs.
There aren’t any additional drug shortages yet, but experts say that generics like painkillersExternal link are particularly vulnerable to disruptions because they are mostly imported from India and China, are subject to high shipping costs, aren’t critical, and yield little financial benefits compared to patented drugs. During the Covid-19 pandemic, Switzerland temporarily limited sales of paracetamol to one box per patient. A similar situation could be possible within months, according to experts.
Restoring energy infrastructures will take several months and FONES has flagged that deliveries of goods to Europe will be delayed regardless of any ceasefire between Iran and the United States.
“You can’t just stop shortages from happening, but you can be prepared”, said Swiss pharmacist Enea Martinelli, who is on the committee of a citizen initiative pushing for a better approach to drug procurement.
Swissinfo looks at the measures Switzerland has implemented to avoid drug shortages and what changes it made after Covid-19, the last global threat to drug procurement.
What measures are currently in place to avoid medicine shortages?
Switzerland has an obligation to stockpile enough essential therapeutic goods, like cancer treatments, painkillers and vaccines, to last five to six months. Since 2015, distributors also have a duty to notify authorities of vital drug shortage risks that could last 14 days or more. A regularly updated list of active substances determine which drugs are considered essential and includes insulin and blood thinners.
But the country has been grappling with drug shortages since the start of the century due to the outsourcing of critical production stages to low-wage countries, a heavy reliance on a small number of production sites in Asia, and the reduction of stock levels throughout the value chain. Despite introducing additional measures since 2006, such as modifying laws so hospitals are better supplied in drugs, global crises like the Covid-19 pandemic or the current conflict in the Middle East systematically exacerbate what FONES says are “fragile and disrupted supply chains”.
What about new measures?
The country is currently modifying its epidemics law, which aims to protect its population from communicable diseases, to give the government more power to intervene. In the event of medical equipment shortages, for example, Bern would be able to step in, instead of only relying on the private sector’s collaboration with cantons, which is how the current system works.
Since 2023, to overcome day-to-day shortages of vital drugs, Switzerland has introduced the reimbursement of drugs prepared by pharmacies, expanded its list of life-saving drugs, and approved fractioned sales of pill boxes. It has also agreed, in some circumstances, to give up on regular assessments that reduce prices of essential drugs to lower healthcare costs. The goal is to give drug manufacturers an incentive to keep those medicines available on the market.
Drug-supply chains are particularly intricate, which means that solutions are particularly difficult to implement. “One shouldn’t expect revolutionary measures because they wouldn’t work”, said Martinelli.
+ Find out how much hope the proposed solutions offer:

More
Five ways health authorities hope to end medicine shortages
Last month, after two years of research, the government presented a proposal to parliament: in the short term, imports from the European Union will be simplified and Swiss-specific multilingual leaflets in medicine boxes will be replaced by QR codes to ease collaboration with products authorised in the EU. By the end of 2026, Switzerland will begin classifying all drugs approved in Switzerland into various categories as opposed to just those that are essential, to determine their use and to track their availability. Until then, drugshortage.ch, set up at Martinelli’s own initiative in 2016, will continue to be the only platform tracking all shortages of drugs.
Some of these measures are already being implemented and in the long term, the country hopes to modify its constitution to give the government additional powers, including modifying laws to give drug manufacturers economic incentives to keep selling certain drugs.
What problems remain?
While measures for life-saving products have been taken, manufacturers aren’t required to flag shortages for drugs that aren’t deemed essential and Switzerland is regularly short of drugs for chronic diseases because it can’t plan ahead. For example, Swiss pharma company Galderma’s powder Nemluvio, which treats severe eczema, has been out of stock since early February. Authorities have authorised the import of an identical product marketed in Germany.
The government’s plan to monitor medication for chronic illnesses comes about ten years too late, according to Martinelli, because it will take several years before it is implemented, as Switzerland’s laws can take several years to pass. “The situation changes very fast for our system to be able to cope with it, and our political system is just too slow,” he said.
Should the Middle East conflict cause further drug shortages, Switzerland would resort to its essential medicines stock. But for drugs that treat chronic diseases, Switzerland has no other choice than to “wait and see” and hope for international collaboration. “We are alone – that’s the problem,” said Martinelli.
Pharma supply chains are a risks for the EU as well, but the difference is that they have a strategy in contrast to Switzerland’s “concept of a plan”, explained Martinelli. France’s strengthening of stock requirement measures in September 2021 is currently being held as a best practice across the 27-member bloc. Some EU countries also have export restrictions, meaning that when a product becomes scarce, it won’t be sold outside the bloc’s borders – thereby cutting out Switzerland.
+ Swiss drug manufacturers’ key European pharma partner

More
Slovenia’s role in the global pharmaceutical supply chain
Switzerland’s Federal Office of Public Health (FOPH) has its own international department, “which maintains regular contact with other international working groups on these issues”, said the FONES spokesperson.
However, Switzerland’s market size will always be a sticking point. “Switzerland is a small market by international standards and is therefore less attractive to companies operating on a global scale, which exacerbates the situation (for example, through companies withdrawing from the market),” the spokesperson added.
Last year, Roche pulled its cancer treatment Lunsumio from the Swiss market because it couldn’t agree on pricing with the national regulator. Meanwhile in Interlaken, a city in canton Bern, vials and perfusion bags producer Bichsel said it would close at the end of the year due to financial difficulties, leaving it up to one company, Streuli, to supply the country with medical equipment central to any treatment, according to local media reportsExternal link.
For Martinelli, fully setting up production lines in Switzerland is not a realistic option for cost reasons, and solving drug shortages will require a paradigm shift from approaching treatments as an economic issue to a therapeutic one. “Nowadays, even if a treatment is very important but is no longer profitable, it would no longer exist in Switzerland,” he said, “and that’s what Switzerland needs to work on.”
Edited by Virginie Mangin/gw

In compliance with the JTI standards
More: SWI swissinfo.ch certified by the Journalism Trust Initiative




























You can find an overview of ongoing debates with our journalists here . Please join us!
If you want to start a conversation about a topic raised in this article or want to report factual errors, email us at english@swissinfo.ch.