
Swiss Alzheimer’s patients find home in Thailand
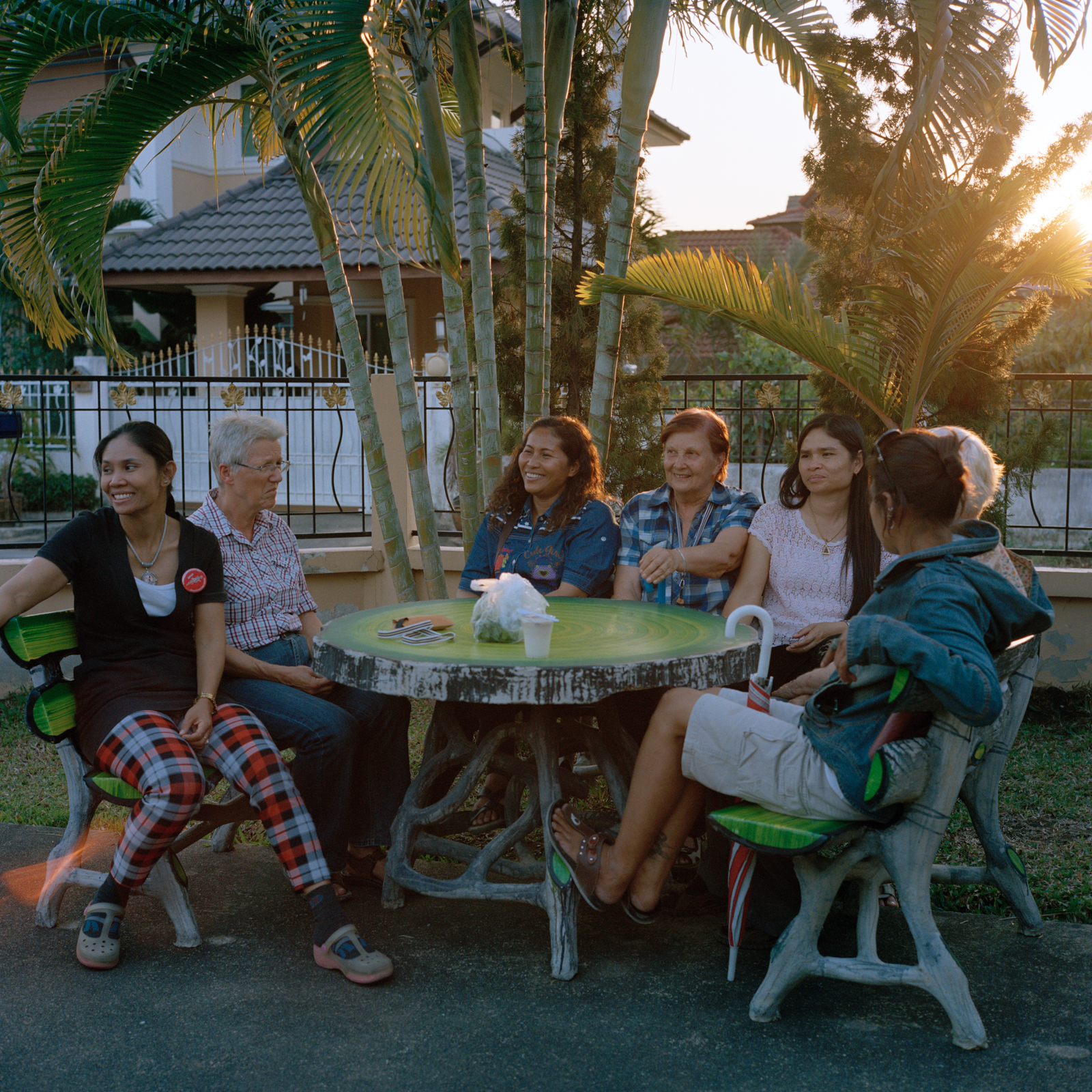
Palm trees and a swimming pool, games and outings – this is not a holiday camp, but a care home for the elderly at Chiang Mai, in Thailand. The Baan Kamlangchay centre, run by a Swiss, accommodates patients with Alzheimer’s and other dementias.
Siegfried Seidel has a problem – the same that many Westerners in Thailand have. He is too tall and always bumps his head against the top of the door frame. For three months, the retired German biologist has been renting an apartment in Faham, a suburb of Chiang Mai, in the north of the country.
Apart from the bruises on his forehead, Seidel is enjoying his holiday. The Buddhist temples and the markets are not what interest him, though. What brought him to Thailand was the illness of his wife, Irene. “In 1999 she was diagnosed with Parkinson’s disease. I tried to put her in a care home in Germany. But she didn’t feel right there, and after four days I took her home,” he recalls.
At their home in Potsdam, the 78-year-old looks after his wheelchair-bound wife on his own. But amid the palm trees of Faham, he has time out to rest and think. He doesn’t have to worry about his wife, as he knows she is in good hands no more than a block away.

More
Why I left my mother in Thailand
Elderly respected in Thailand
Irene Seidel is a guest at Baan Kamlangchay, a residence for people suffering from Alzheimer’s disease and other senile dementias. The centre offers stays of varying duration to patients from Switzerland and Germany. “I wanted others to benefit from my experience,” explains founder Martin Woodtli.
In 2002, after his father died, the psychotherapist from Münsingen, outside Bern, was left to care for his mother, who was suffering from Alzheimer’s. Putting her in a normal care home was not an option for Woodtli. He did not want his mother, who was hyperactive, to be limited in her movements and kept sedated with lots of medication. Permanent care in Switzerland was not an option financially either. So he decided to “follow his heart” and make the journey with his mother to Thailand, which is a country he knows well, as he worked here at one time with Médecins Sans Frontières.
The cost of living and the lower wage bill here are not the only argument for the offshore solution. “In Thailand the elderly enjoy great respect,” emphasises Woodtli. “It is considered normal that younger people take care of them.” His positive experience with local caregivers who looked after his mother around the clock convinced him of the rightness of the decision he had made. A year later he founded Baan Kamlangchay.
“Here I can recharge my batteries,” says Siegfried Seidel. “At home, apart from looking after Irene day and night, I am always afraid of making a wrong move or falling. If I broke an arm or a leg, who would look after her?”

More
A lifetime’s memories erased
Three caregivers per patient
Beside the centre’s swimming pool, in the shade of a pavilion, a group of elderly people are at play, throwing each other a large blue ball. Judging from the laughter, this is a favourite activity enjoyed not only by the patients but by the Thai nursing staff as well. At Baan Kamlangchay it is often the Parkinson’s and Alzheimer’s patients – at least those who are still mobile – who decide what to do.
Because the elderly patients are free to move around, they receive constant care on an individual basis. Each patient is looked after by three caregivers, who take turns accompanying him or her in every activity. At night, there is always someone sleeping in the same room. “In Switzerland this wouldn’t be feasible,” notes Ursula Lanz, a specialist in geriatrics and psychiatry who is volunteering for a month in Faham. The relationship with the care staff, she emphasises, “is crucial for dementia patients. You won’t get the same result if there is just one nurse for seven or eight patients.”
Living thousands of miles from home and encountering a different language and culture does not seem to be a major problem for the residents. “In the advanced stages of dementia, as we have here, the language is not that important,” says Lanz. Taking the place of words are gestures, looks, facial expressions and touch. The patients bring their life stories and their memories here with them, says Woodtli, who recalls how his mother, who has since died, used to walk around the streets of Chiang Mai thinking she was in Bern.
On the other hand, the atmosphere at Baan Kamlangchay is not entirely exotic. There is Swiss food – breakfast includes muesli, bread and café au lait – and popular songs in German can be heard playing in the background.
Placing Alzheimer’s patients in a specialised clinic in Thailand may be a solution, but only in certain cases, cautions the Alzheimer’s Association of Switzerland.
Asians, the organisation states, have a reputation for treating elderly people with great respect and accepting the effects of aging. Furthermore, in Thailand, lower wages mean you can afford to hire more people for individualised care.
However, this option is only indicated for a minority of patients; that is, for those who already know the country, says the association’s director, Birgitta Martensson.
“Having spent two weeks’ holidays there is not enough. There must be good reason to believe that the patient will feel well there over the long term,” she told swissinfo.ch.
“Alzheimer’s patients need their nearest and dearest around them. They need to feel safe and surrounded by familiar things.”
According to Martensson, there is no evidence that location and verbal communication are not important for the patient. An unfamiliar environment may cause increasing disorientation.
“Surely a person should be able to stay in his own home country and not be ‘exported’ as if he was an undesirable,” she insists. Switzerland, she believes, should make more resources available for care staff, who are too few in number and often get little training, so they can help patients living at home.
Alternative solutions for dementia
Baan Kamlangchay remains a somewhat unusual alternative for dementia patients and their family members, and it does not appeal to everyone.
The Alzheimer’s Association of Switzerland recognises that having patients cared for abroad is a feasible option. Yet taking a person far away from the place they have known and lived in for a lifetime may have adverse consequences, the organisation cautions (see info box).
On the other hand, the Thai people, who are very family-conscious, have been slow to understand the choices made by the families from overseas with elderly patients at Baan Kamlangchay. “I wondered how people could abandon their parents in Thailand,” says a local woman who runs a food store in Faham. “Then I thought that they could not look after them because of work.” But at this point, she says, the patients at Baan Kamlangchay have become part of everyday life in the small town.
Integration in the social setting is one of the most important aspects of patient care for Woodtli. For that reason he accommodates the residents in six houses scattered around the neighbourhood. Although he fields inquiries on a daily basis, he does not intend to expand the operation. “We are a family business and we need to stay that way.”
Since 2003, the centre has accommodated about 70 people. The stay in Thailand costs CHF3,500 per month – a third of what it might cost in a home in Switzerland. Money should not be the deciding factor, however, cautions Woodtli. “If I get the feeling that people are bringing us dementia patients just because of cost considerations, I turn them down,” he says.
In Switzerland it is believed that persons suffering from Alzheimer’s or another form of dementia number over 110,000 (with a world total of about 36 million people). The number could increase to 200,000 by 2030 and to 300,000 by 2050.
Dementia affects 8% of people over 65 and 30% over those over 90.
Six patients out of ten live at home. Of these, half need help every day and 10% need round-the-clock attention.
Overall, costs of dementia in Switzerland amount to about CHF 7 billion per year (with CHF20 billion projected for 2050).
An Alzheimer’s patient lives on average 8–10 years. Currently there are no therapies to cure or slow down the course of the illness.
Source: Alzheimer’s Association of Switzerland
A growing problem
No one really knows how to deal with the increase in the number of cases of dementia in the Western world, Woodtli notes. In Switzerland, it is expected that the number of people with Alzheimer’s will double by 2030. There is an urgent need to find alternatives, new models of care. “I chose Thailand on account of my own past experience,” Woodtli says. “But it could be done elsewhere, including Europe.”
The essential thing, he says, is to provide the human contact which the patients need. Major residential care projects, like some now growing around Chiang Mai, he regards with scepticism. They risk losing the family atmosphere and repeating bad experiences in Switzerland and Germany where there is not enough time for the patients.
Time is a precious commodity for Siegfried Seidel. His holiday will soon be over. He will be leaving Faham and the beautiful orchids he has been growing in the garden. But leaving his wife permanently here in Thailand, as some others have done, is something he does not want to consider. “We have been married 59 years,” he says. “We have been through good times and bad times together. I’m not going to abandon her now.”
(Translated from Italian by Terence MacNamee)

In compliance with the JTI standards
More: SWI swissinfo.ch certified by the Journalism Trust Initiative
































You can find an overview of ongoing debates with our journalists here . Please join us!
If you want to start a conversation about a topic raised in this article or want to report factual errors, email us at english@swissinfo.ch.