
Treating mental illness in pregnancy ‘still a grey area’
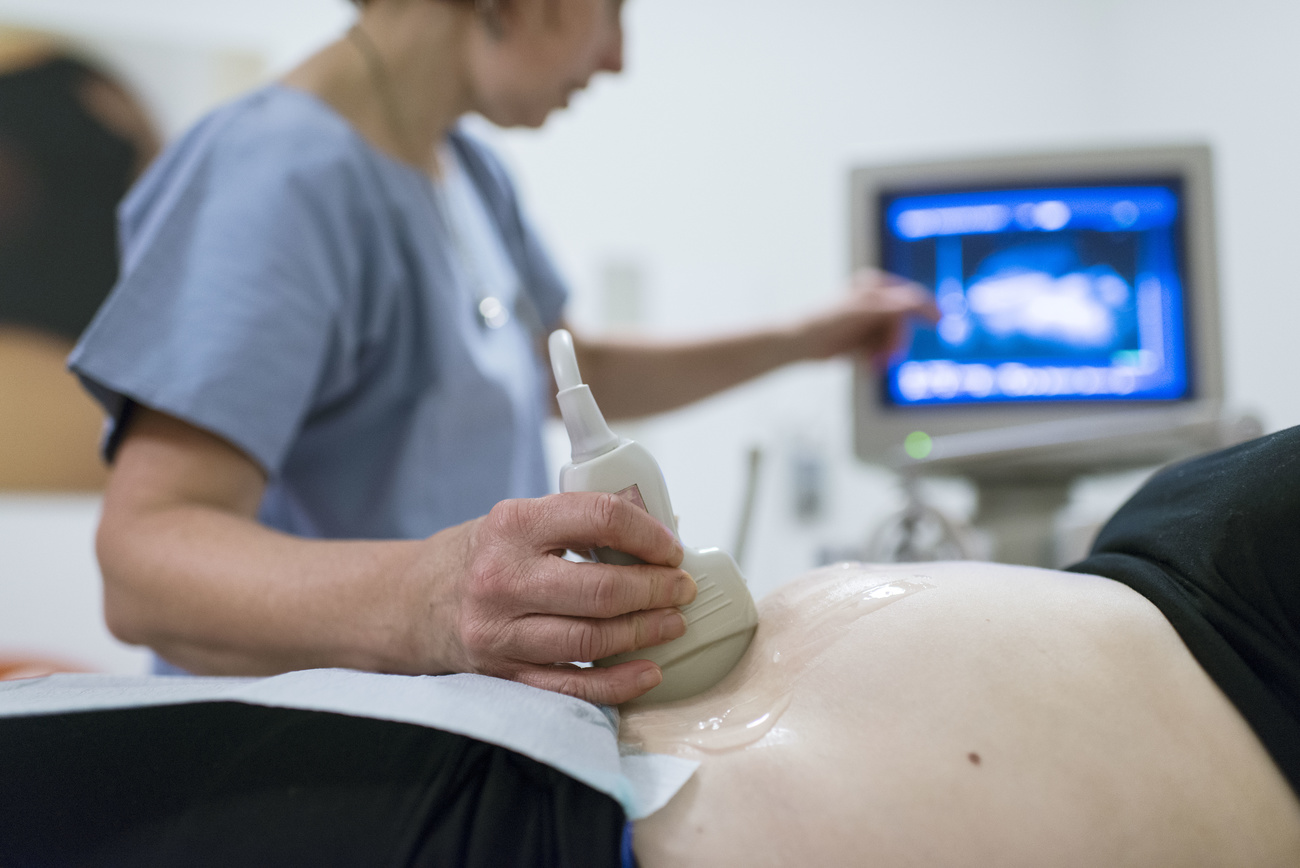
The lack of research data on pregnant women means there is no global standard of care for expectant mothers with a history of mental illness, experts have said. With one in ten pregnant women experiencing depression, the problem should be too large to ignore.
Their comments came ahead of an International Forum of Women’s Brain and Mental Health, which will be held by webcast by the Swiss-based Women’s Brain ProjectExternal link this weekend (swissinfo.ch is a media partner of the forum.)
The relapse rate of women with psychiatric disorders who stop their medications during pregnancy is extremely high, said psychiatrist Jennifer Payne of the Johns Hopkins Women’s Mood Disorders Center in BaltimoreExternal link, in a special online panel discussion held before the forum. She will also be attending the forum remotely.
The expert panel on maternal mental health is part of the third International Forum on Women’s Brain and Mental Health organised by the Women’s Brain Project (WBP). The Forum webcast takes place on September 19 – 20.
The Women’s Brain Project (WBP) is an international non-profit organisation based in Switzerland. Composed largely of scientists, WBP advocates for and conducts research on sex and gender sensitive precision medicine, from basic science to novel technologies.
The author will moderate a live panel discussion on maternal mental health on September 19. swissinfo.ch is also a media partner of the forum.
“In women with major depression, 70 per cent will relapse during pregnancy and this increases to 85 per cent or more in bipolar disorder,” Payne said.
The relapse rate in women who continue their medication is also high – one in four for major depression and one in three for bipolar disorder.
According to Sergio PecorelliExternal link of the University of Brescia and Yale University, another panel participant, the literature has two important challenges. One is a lack of trial data which leads to a reliance on observational data. The other is the narrow range of conditions and medications that are studied.
“Unfortunately, this really is a grey area, especially in the world of research about medication and also if we look at the regulatory agencies to see if drugs have been tested during pregnancy.”
Damned if you do…
The medical profession is understandably nervous about causing harm to pregnant women. “But I would argue that we are causing harm by not having the data we need to guide treatment. We treat all kinds of medical conditions in pregnancy from asthma to cancer and there’s no question that we should treat those conditions,” Pecorelli said.
Payne made the point that mood stabilising medication is no more optional than epilepsy medication, for example. “I think it is the stigma against psychiatric disorders that is driving the message to women to stop their medications during pregnancy,” she said.
One of the reasons for the high relapse rate in psychiatric disorders for women during pregnancy, even for women who continue their medications, is that there are massive changes in metabolism, body weight and blood volume during pregnancy that can affect efficacy of medications, she explained.

More
Swiss non-profit aims to break taboo of women’s brain health
“Pregnant women deserve an evidence base for the prevention and treatment of their illnesses equal to others as a matter of justice,” Payne said. There have been limitations on involving pregnant women in Covid-19 vaccination research as well.
There may be some lessons to be learned from the approach in neurology. “Epileptic medications are prophylactically adjusted based on plasma levels for women with seizure disorders. Maybe we could prevent that high rate of relapse in women who continue their meds if we were monitoring blood levels, adapting prophylactically and tapering the medication prior to delivery,” she added.
But the lack of data is a major hindrance. “The reality is we have not done the studies that we need to determine the proper management of medications during pregnancies.”
More
Life-changing
Pregnancy can also be when mental disorders emerge for the first time, partly triggered by hormonal influences. In her contribution to the discussion, Franka Cadée, President of the International Confederation of Midwives,External link stressed that pregnancy and childbirth are life-changing events.
“It’s common for women to feel more anxious or a bit down at this time and some may develop depression or other mental health problems. On the other hand, some women with a history of severe mental illness remain well during pregnancy.”
The important thing is to remember that everyone is different and to adapt their care accordingly, she said.
Swiss experts acknowledge that the situation is not straightforward and need a high level of care. Daniel Surbek of the Insel hospital in Bern, is a leading Swiss expert on fetomaternal medicine. “The conditions of pregnant women with psychiatric or addiction disorders are complex and demand an individual risk assessment and the adaptation of the psychopharmacotherapy [medication],” he wrote in a recent paper on the care of pregnant women with psychiatric illnesses.
In Surbek’s experience, the favourable effects of continuing medication often outweigh the negative effects. “Ultimately, you have to strike a balance.”
Balance
Pecorelli spoke about this balance, recalling that the beginning of life is very important for mental health, even including pre-conception through parental environmental exposures.
“All currently available psychopharmacological agents and their metabolites [a substance produced during or taking part in metabolism] cross the placenta. Some medications can affect the foetus,” he said.
But an ill mother also affects the foetus – and there’s the rub. Stress hormones and other physiological consequences of depression and anxiety are picked up by the developing foetus.
After birth, very young infants are highly sensitive to the environment and the quality of careExternal link. Pecorelli echoed the point made by other panellists that depressive symptoms in mothers can interfere with responsive caregiving and are associated with a range of psychological and developmental disturbances in children.
More
How ‘men as default humans’ threatens to undermine precision medicine
In Switzerland, expectant mothers with mental health issues are well provided for. According to Surbek, prenatal care in such complex and demanding cases “requires interdisciplinary cooperation between psychiatrists, gynaecologists and obstetricians, ideally in a specialised centre to achieve the best outcome for mother and child”.
Meanwhile, in many low- and middle-income countries, access to essential medicines for mental disorders remains a major challenge.
Stressors and prevention
Pregnancy doesn’t happen in a vacuum. The question has to be asked, why is a woman depressed and what can be done about it? Social risk factors such as insecure housing, poverty and gender-based violence can be just as significant as biological risk factors, experts said.
The rate of perinatal mental health problems is three to five times higher for women exposed to partner violence, Cadée observed.
Stressors during pregnancy are also associated with the onset of neurological disorders in the offspring. The first paper that came out on this examined the impact of the German invasion of the Netherlands in the 1940s. It looked at outcomes for babies of mothers pregnant at that time. In later life these children had a much higher rate of schizophrenia, for instance.
The current situation with Covid-19 has also become a stressor, adding more challenges to maternal mental health. Social isolation may affect women’s access to their social support networks and reduce access to some types of medical support.
The risks appear numerous and overwhelming but Cadée concluded the panel discussion with a strong but simple message: “Prevention is extremely important. If we want to take women seriously, we have to dare to listen to their needs and act accordingly. Women often know what they need. It is a matter of listening.”

In compliance with the JTI standards
More: SWI swissinfo.ch certified by the Journalism Trust Initiative




























Join the conversation!