
Swiss help developing nations combat fake drugs
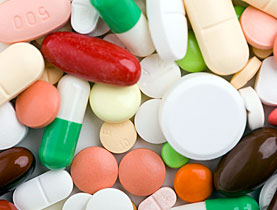
A team of Swiss engineers and pharmacists has built a low-cost machine, due to be launched in Mali, aimed at helping poor countries detect counterfeit medicines.
Fake drugs are a growing public health problem, especially for developing nations. The World Health Organization (WHO) says over 30 per cent of medicines sold in many African countries, as well as parts of Asia and Latin America, may be counterfeit.
According to the US-based Centre for Medicines in the Public Interest, counterfeit drug sales will reach $75 billion (SFr77.1 billion) globally in 2010, an increase of more than 90 per cent compared with 2005.
Counterfeiting is greatest in those regions where medicines’ regulatory and enforcement systems are weakest. In Africa, where almost 80 per cent of drugs are imported, fake drugs and the lack of means to analyse their quality can have catastrophic consequences.
The WHO says at least 200,000 lives could be saved every year if there were no fake medicines. In 2008 more than 80 babies in Nigeria died from teething medicine that contained the toxic coolant diethylene glycol.
To help prevent such illnesses and deaths, the Geneva-Lausanne School of Pharmacy, together with the Fribourg College of Engineering and Architecture, have come up with a unique quality-control solution for developing countries.
Their aim was to design a tool that was cheap, simple, sturdy and able to cope with extreme weather conditions.
The low-cost analytical device uses capillary electrophoresis, a recognised technique which separates molecules by size and electrical charge.
Low cost
“The technique is extremely interesting as it uses little material and has a low analytical cost, but it’s not that well known,” Serge Rudaz, project coordinator at Geneva’s School of Pharmacy, told swissinfo.ch.
Such instruments already exist on the market but are extremely expensive – SFr60,000-80,000 ($58,400-78,000) – and are difficult to maintain. The new machine costs only SFr8,000.
After three years’ development the bright-red instrument will be sent in early November to the National Health Laboratory at Bamako University in Mali, which has special cooperation agreements with Geneva University.
Swiss engineers will travel to Bamako to set up the device and train colleagues from Mali to guarantee the project’s longevity, Rudaz explained.
Counterfeit drugs are a major problem in Mali. Many are imported from India and China, where production conditions don’t always meet international pharmaceutical standards. Mali’s extreme weather conditions can also cause badly stored drugs to deteriorate.
Bamako laboratory
The National Health Laboratory’s existing methods for detecting counterfeit medicines are expensive and technically demanding. The laboratory has growing difficulties in obtaining reasonably priced high-quality organic solvents, for example.
The new machine, which uses a tiny amount of solvent and small quantities of water in the analysis process, is much simpler to operate and maintain, according to Rudaz.
In the development phase the apparatus was tested on a selection of 20 well-known drugs, including Amoxicillin, used to treat bacterial infections, the antibiotic Cotrimazol, HIV antiretroviral treatments and Quinidine, an anti-malarial drug.
“But in principle it can test any kind of drug,” he said.
The scientists are already banking on the success of their project and have set up an association, Pharmelp, to be able to propose their low-cost drug control approach to other developing countries.
Rudaz is certain that word of mouth in the African medical world will ensure its success. In the meantime he has already been contacted by interested partners from Madagascar and Cambodia.
Simon Bradley, swissinfo.ch
According to the US-based Centre for Medicines in the Public Interest, counterfeit drug sales will reach $75 billion (SFr77.1 billion) globally in 2010, an increase of more than 90 per cent from 2005.
Officials do not suspect counterfeit drugs are being made in Switzerland but that the country serves as a transit point.
Often a counterfeit drug may appear to come from a European country when in fact the online operation may be based in Africa and the labs in Asia. Most believe criminal organisations are behind the sales.
The problem of counterfeit medicines was first addressed at the international level in 1985 at the WHO Conference of Experts on the Rational Use of Drugs in Nairobi. Since then WHO has adopted a number of resolutions to deal with the issue and in 2006 it launched an international anti-counterfeiting taskforce (Impact).
But getting governments and law enforcers around the world to work more effectively to counter the problem has proved hard.
But that may be changing. On October 11, 2009 former French President Jacques Chirac launched an initiative to combat counterfeit medicines. The so-called “Cotonou Declaration” is the first step of a worldwide campaign aimed at raising awareness of the problem and persuading governments to impose tougher penalties and improve routine testing of medications. The larger goal is to establish an international convention on counterfeit drugs as early as next year.

In compliance with the JTI standards
More: SWI swissinfo.ch certified by the Journalism Trust Initiative

























You can find an overview of ongoing debates with our journalists here . Please join us!
If you want to start a conversation about a topic raised in this article or want to report factual errors, email us at english@swissinfo.ch.